Suraj kumar1*, Gowrishankar Potturi1, Rajkumar2, Neha Dubey1, Anjali Agarwal1, Arushi Kumar3
1Department of Physiotherapy, Faculty of Paramedical sciences, Uttar Pradesh University of Medical Sciences, U.P, India
2Vice-chancellor, Uttar Pradesh university of Medical Sciences, Uttar Pradesh, India
3Medical Researcher, Uttar Pradesh, India
*Corresponding author: Suraj Kumar, Associate Professor & Head, Department of Physiotherapy, Faculty of Paramedical sciences, Uttar Pradesh University of Medical Sciences, Saifai, Etawah, U.P, India
Received: 09 July 2020; Accepted: 18 July 2020; Published: 06 August 2020
COVID-19 pandemic mostly affects respiratory system resulting in cough, sputum production, dyspnoea, hypoxemia as in pneumonia. Currently, 5 % of COVID-19 cases require admission to ICU due to respiratory distress. The global current treatment options mostly followed for ARDS due to COVID-19 pneumonia include high flow nasal canula (HFNC), non-invasive ventilation (NIV), mechanical ventilation with lower tidal volumes and continuous positive airway pressure (CPAP). There is high risk of aerosol dispersion during these techniques provoking the risk of cross infection, as most of the COVID-19 hospitals are not having negative pressure isolation rooms. There is also an acute shortage of mechanical ventilators globally. Short Wave Diathermy is a physical therapy antibiotic which has antimicrobial effects, possessing the capacity to reduce cyanosis, pain, dyspnoea, cardiac embarrassment and induces restful sleep. Short wave diathermy with acute precautionary measures could be beneficial in reducing the temperature, improving circulation, reducing respiratory rate, grunt and Pain.
COVID-19, Pneumonia, Short Wave Diathermy, Physical Antibiotic
1. Introduction
COVID-19 disease caused by corona virus shows early patterns a trend similar to Severe Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS) [1]. COVID-19 often shows pneumonia like symptoms like hypoxemia, cough (68%), sputum production (34%) and shortness of breath (19%) [2]. Approximately, 5 % of COVID-19 cases require admission to ICU due to respiratory distress [3]. According to the Berlin definition of ARDS, it is a specific disease, with distinctive features of severe hypoxemia associated with near normal respiratory system compliance. The most common patterns of COVID-19 pneumonia are Type -L characterized by Low elastance, Low ventilation to perfusion ratio, Low lung weight and Low recruitability. The second pattern being Type H appertaining to High elastance, High right to left shunt, High lung weight and High recruitability [4, 5]. The COVID-19 pneumonia pattern depends on interaction between the severity of infection, host response, physiological reserve, comorbodities, ventilator responsiveness of the patient to hypoxemia, time between onset of disease and intervention.
The Biomarkers play an important role in diagnosis and prognosis of Pneumonia and are now considered as gold standards in medicine. The common biomarkers used to detect the pneumonia are C-reactive protein, Leucocytes count, immunoglobulin and pro-inflammatory cytokines etc [6, 7, 8]. The global current treatment options mostly followed for ARDS due to COVID-19 pneumonia is High flow nasal canula (HFNC), continuous positive airway pressure (CPAP), non-invasive ventilation (NIV), mechanical ventilation with lower tidal volumes [5, 9]. Nearly 5 % of cases require mechanical ventilation which is now an endemic in the developing world [10]. A high flow nasal canula or non-invasive ventilation is not recommended till viral clearance [11].
There is high risk of aerosol dispersion during these techniques provoking the risk of cross infection, as most of the COVID-19 hospitals are not having negative pressure isolation rooms [12]. Apart from the cross infection, non-invasive ventilation in pneumonia patients temporarily improves oxygenation, reduces work of breathing but doesn’t change the natural disease course [13]. Short wave diathermy (SWD) is a deep tissue heating modality that exerts therapeutic effects by using electromagnetic radio waves at a frequency of 27.12 MHz [14, 15] and 11m wavelength. It provides both thermal and non thermal effects where the non thermal effects of SWD are based on low dose (Oligothermic) [16]. The production of non-thermal effects is due to the vibrations induced to the tissue molecules when exposed to the radio waves [17, 18]. SWD has been used to treat severe respiratory infections like pneumonia before the invention of antibiotics. The diathermy is believed to increase the white blood cell count, blood flow to the area. It also detoxifies the liver [19].
2. Methodology
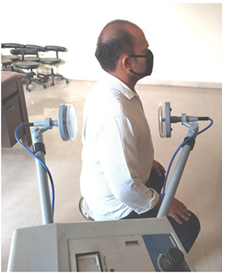
The pneumonia cases are diagnosed using the Biomarkers as a gold standard. The best identified protocol for delivering SWD in pneumonia patients was recommended by Jan Zbigniew Szopinski (2014) in the paper reflexive physical therapies postulated the protocol for treating chronic obstructive pulmonary diseases. The condenser electrodes place at a distance of 4 cm from the treated region for duration of 15-20 min by contra planar method. The electrodes are placed parallel on opposite planes, in pneumonia they are placed on anterior and posterior aspects of Chest wall (Figure 1). The recommended dosage is described as oligothermic, very mild thermal sensations to hyperthermic, strong but not unpleasant sensations [20].
3. Discussion
The bio- thermal therapy [21] which uses deep tissue heating for various clinical conditions is a research based approach which dates back 200 years ago. SWD is frequently used in infections and has a century back long track record of improving infection guidelines. It is frequently called as "physical therapy antibiotic". It has a track record of reducing 50% death rate in pneumonia and doubling the recovery rates. In the corona virus naturopathic guidelines (COVID-2019), Portland clinic of Holistic Health, recommended the use of Short wave diathermy in COVID-19 pneumonia to combat the infection and inflammation of the lungs, reduce mortality and enhance recovery [22]. The benefits of SWD on the Pneumonia were first recognized by Frederick DeKraft and Byron Sprague Price, of New York, about the year 1906.
In 1921, there was a severe Pneumonia epidemic in U.S. marine Hospital, New York, a study was conducted on 41 patients with radiologically and laboratory diagnosed pneumonia cases, where 20 cases were given SWD and 21 were controls. The death rate was 17 % in experimental, i.e. SWD group compared to 42 % in control group [23]. From the above study, the established physiological effects of SWD in pneumonia patients are as follows [24]:
- Temperature: There was a drop of temperature resulting in conserving body energy, reducing pulse and respiratory rate.
- Circulation: there was a lessening of cyanosis and was more evident when lower lobes are affected. This effect is due to decrease in pain and improvement in the intrapulmonic circulation around the consolidated areas. It decreased the load on the right ventricle, resulting in improvement in the quality of pulse.
- Respiration: The respiratory rate was reduced by an average of five per minute and respiratory grunt disappeared. All these effects are contributed to improved pulmonary circulation in response to heat.
- Pain: There was reduction in pain resulting in reduced anxiety levels and improved respiratory efforts.
A maximum of six to eight treatment sessions with SWD showed marked reduction in the size of inflammation and pulmonary opacity in radiographs. SWD applied through the chest in pneumonia patients provides a sense of well being by dues ex machine principle. It has also shown to reduce bronchospasm, general relaxation and reduction in the viscosity of mucous aiding in proper drainage [25].
4. Conclusion
SWD is a physical therapy antibiotic which has antimicrobial effects, possessing the capacity to reduce cyanosis, pain, dyspnoea, cardiac embarrassment and induces restful sleep. The use of SWD in treating pneumonia has been successful since 1906. In the present pandemic COVID-19, where 5 % of the cases need mechanical ventilation due to development of pneumonia like symptoms, SWD can be given at oligothermic dosages to combat the infection and respiratory distress. As there is global shortage of ventilator, a risk of aerosol dispersion cross infection, Short wave diathermy with acute precautionary measures could be beneficial in reducing the temperature, improving the circulation, reduction in respiratory rate and grunt, Pain. SWD may be included for RCT to study the effect of the cases of COVID pneumonia.
Acknowledgement
The authors acknowledge the authorities of Uttar Pradesh University of Medical Sciences, Saifai, Etawah, Uttar Pradesh for approval and encouragement
Source of Funding
NIL
Conflicts of Interest
The authors declare no conflicts of Interest
References
- Fehr AR, Channappanavar R, Perlman S. Middle East respiratory syndrome: emergence of a pathogenic human coronavirus. Annu Rev Med 68 (2017): 387-399.
- Chavez S, Long B, Koyfman A, et al. Coronavirus Disease (COVID-19): A primer for emergency physicians. Am J Emerg Med S0735-6757(2020): 30178-30179.
- Guan WJ, Ni ZY, Hu Y, et al. Clinical Characteristics ofCoronavirus Disease 2019 in China. N Engl J Med (2020).
- Zhu N, Zhang D, Wang W, et al. A Novel Coronavirus from Patients with Pneumonia in China, 2019. N Engl J Med 382 (2020): 727-733.
- Luciano Gattinoni, Davide Chiumello, Pietro Caironi, et al. COVID-19 pneumonia: different respiratory treatment for different phenotypes?. Intensive Care Medicine 46 (2020): 1099-1102.
- Christ-Crain M, Opal SM. Clinical review: the role of biomarkers in the diagnosis and management of community-acquired pneumonia. Crit Care 14 (2010): 203.
- Faix JD. Biomarkers of sepsis. Crit Rev Clin Lab Sci 50 (2013): 23-36.
- Karakioulaki M, Stolz D. Biomarkers in Pneumonia-Beyond Procalcitonin. Int J Mol Sci 20 (2019): 2004.
- Gattinoni L, Caironi P, Cressoni M, et al. Lung recruitment in patients with the acute respiratory distress syndrome. The New England journal of medicine (2006).
- Cascella M, Rajnik M, Cuomo A, et al. Features, Evaluation and Treatment Coronavirus (COVID-19). In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing (2020).
- Krishnamoorthy Vijay, Vavilala Monica S, Mock Charles N. "The need for ventilators in the developing world: An opportunity to improve care and save lives". Journal of Global Health. 4 (2014): 010303.
- Cheung J C-H, Ho LT, Cheng JV, et al. Staff safety during emergency airway management for COVID-19 in Hong Kong. Lancet Respir Med (2020).
- Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) in China. Zhonghua Liu Xing Bing Xue Za Zhi 41 (2020): 145-151.
- Goats GC. Continuous short-wave (radio-frequency) diathermy. Br J Sports Med 23 (1989): 123-127.
- Ozen S, Doganci EB, Ozyuvali A, et al. Effectiveness of continuous versus pulsed short-wave diathermy in the management of knee osteoarthritis: A randomized pilot study. Caspian J Intern Med 10 (2019): 431-438.
- Al-Mandeel MM, Watson T. The thermal and nonthermal effects of high and low doses of pulsed short wave therapy (PSWT). Physiother Res Int 15 (2010): 199-211.
- Romanenko S, Begley R, Harvey AR, et al. The interaction between electromagnetic fields at megahertz, gigahertz and terahertz frequencies with cells, tissues and organisms: risks and potential. J R Soc Interface 14 (2017): 20170585.
- Kim JH, Lee JK, Kim HG, et al. Possible Effects of Radiofrequency Electromagnetic Field Exposure on Central Nerve System. Biomol Ther (Seoul) 27 (2019): 265-275.
- Namendys-Silva SA, Hernández-Garay M, Rivero-Sigarroa E. Non-invasive ventilation for critically ill patients with pandemic H1N1 2009 influenza A virus infection. Crit Care 14 (2010): 407.
- De Cholnoky T. Short-wave Diathermy. New York: Columbia University Press (1937).
- Huang Huang-Wen, Liauh Chihng-Tsung. Heating in Biothermal Systems (2011).
- Jan Zbigniew Szopinski. Reflexive Physical therapies. The Biological Action of Physical Medicine (2014).
- Portland Clinic of Holistic Health Updated 03/02/20 EB Patient Handouts, Corona Virus Detailed Response 03012020.
- Stewart HE. Diathermy in the Treatment of Pneumonia. Proc R Soc Med 19 (1926): 53-56.
- Blackwood S. "Shortwave diathermy (S.W.D.) in the treatment of unresolved pneumonia." South African Journal of Physiotherapy [Online] 36.3 (1980): 72-73.