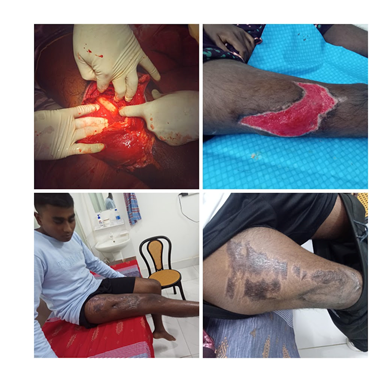
Mohammed Gulam Mustofa1*, Avishek Bhadra2, Sushmoy Saha3, Sabbir Ahmed3, Ashikur Rahman4
1Associate Professor, Department of Orthopaedics, President Abdul Hamid Medical College Hospital, Kishoregonj, Bangladesh
2Assistant Professor, Department of Orthopaedics, President Abdul Hamid Medical College Hospital, Kishoreganj, Bangladesh
3Assistant Registrar, Department of Orthopaedics, President Abdul Hamid Medical College Hospital, Kishoreganj, Bangladesh
4Indoor Medical Officer, Department of Orthopaedics, President Abdul Hamid Medical College Hospital, Kishoreganj, Bangladesh
*Corresponding Author: Mohammed Gulam Mustofa, Associate Professor, Department of Orthopaedics, President Abdul Hamid Medical College Hospital, Kishoregonj, Bangladesh.
Received: 18 February 2025; Accepted: 24 February 2025; Published: 05 March 2025
Background: Degloving injuries, particularly those complicated by jaundice and septicemia, pose significant clinical challenges due to their complex nature and high risk of morbidity and mortality. This study evaluates demographic, clinical, and management factors affecting outcomes in patients with such injuries in a resource-limited setting in Bangladesh.
Methods: A prospective observational study was conducted at the President Abdul Hamid Medical College Hospital, Kishoreganj, Bangladesh, from January 2023 to December 2024. A total of 40 patients with degloving injuries and associated systemic complications were included. Data were collected on demographics, injury characteristics, management strategies, and outcomes, and analyzed for significant associations with mortality.
Results: The majority of patients were male (80%) and aged 31–45 years (45%), with road traffic accidents being the most common cause (50%). Vascular compromise was observed in 70% of cases, and septicemia severity was moderate in 50% of patients. Management strategies included debridement and primary closure (50%), skin grafting (37.5%), and flap reconstruction (12.5%). The survival rate was 87.5%, with full functional recovery achieved in 50% of survivors. Mortality was significantly associated with age >45 years, SOFA scores >10, severe jaundice, and delayed hospital admission.
Conclusion: This study underscores the importance of early intervention, effective infection control, and comprehensive systemic management in improving outcomes for degloving injuries with systemic complications. Context-specific strategies are critical for addressing these challenges in resource-limited settings.
Degloving injuries; Jaundice; Septicemia; SOFA score; Mortality
1. Introduction
Degloving injuries represent a severe form of traumatic injury characterized by the avulsion of skin and subcutaneous tissue, leading to extensive exposure of underlying structures such as muscles, tendons, and bones. These injuries, though rare, are devastating due to the significant tissue loss and high risk of complications, including vascular compromise, infection, and systemic conditions like septicemia and jaundice. The global prevalence of degloving injuries is challenging to quantify due to underreporting, especially in low- and middle-income countries (LMICs) where these injuries are often associated with occupational hazards and high-energy trauma events such as road traffic accidents (RTAs) and agricultural machinery accidents [1,2]. In LMICs like Bangladesh, the public health implications of degloving injuries are profound, given the limited availability of specialized care, delays in accessing healthcare, and socio-economic constraints that exacerbate outcomes [3]. The clinical management of degloving injuries is inherently complex, requiring a multidisciplinary approach to address both local wound care and systemic complications. These injuries often result in significant vascular compromise and tissue necrosis, creating an ideal environment for bacterial proliferation and subsequent septicemia, a systemic inflammatory response to infection. The addition of jaundice, often indicative of underlying hepatic dysfunction or hemolysis, further complicates the clinical picture and significantly increases morbidity and mortality [4,5]. Studies have reported high mortality rates in patients with such complications, underscoring the need for prompt and comprehensive management strategies [6]. The high rates of disability and mortality observed in patients with degloving injuries complicated by jaundice and septicemia highlight the urgency of addressing these interrelated conditions [4,7]. Epidemiological data from Bangladesh indicate that trauma-related injuries, particularly RTAs, are a leading cause of morbidity and mortality. Rural and industrial regions are disproportionately affected, where manual labor and high-risk occupations expose workers to machinery accidents and falls, both of which are major causes of degloving injuries [8,9]. For instance, in rural Bangladesh, road accidents are responsible for up to 30% of injuries, and agricultural machinery contributes significantly to workplace accidents, highlighting the vulnerability of the rural workforce [10]. These injuries are further compounded by systemic socio-economic barriers, including lack of access to timely medical care, inadequate emergency response systems, and financial constraints that delay or prevent treatment [9,11]. Despite this burden, trauma care infrastructure in Bangladesh remains underdeveloped, with a lack of specialized centers and trained personnel, particularly in rural areas [12]. Addressing degloving injuries in Bangladesh is particularly critical given the prevalence of high-risk occupations and the limited healthcare resources available. Inadequate triage protocols, a shortage of essential medical supplies, and financial barriers exacerbate the already poor outcomes for patients with these injuries [13]. Furthermore, the lack of a standardized approach to managing degloving injuries complicated by systemic conditions like septicemia and jaundice underscores the need for context-specific research to guide clinical practice and policy. There is a pressing need for strategies that integrate advanced surgical techniques, such as grafting and reconstructive procedures, with rigorous infection control and systemic management of complications [5,6,14]. Such approaches could significantly improve patient outcomes and reduce the socio-economic burden of these injuries. This study aims to evaluate comprehensive management strategies for degloving injuries complicated by jaundice and septicemia within the context of Bangladesh’s healthcare system. By exploring the challenges and outcomes associated with these cases, the study seeks to provide actionable insights into improving clinical care and addressing gaps in trauma management. Through this research, we hope to contribute to the development of evidence-based protocols that enhance survival rates, functional recovery, and quality of life for patients suffering from these devastating injuries in resource-limited settings.
2. Methods
This study was conducted at the President Abdul Hamid Medical College Hospital in Kishoreganj, Bangladesh, over a period of nearly two years, from January 2023 to December 2024. A total of 40 patients presenting with degloving injuries complicated by jaundice and septicemia were included in the study. Patient selection was based on clinical diagnosis of degloving injuries with associated systemic complications, confirmed through detailed medical history, physical examination, and relevant laboratory investigations. All patients were managed according to a standardized protocol incorporating surgical intervention, infection control measures, and systemic management tailored to the complications of jaundice and septicemia. Data on patient demographics, injury characteristics, clinical management, and outcomes were collected prospectively. Ethical approval for the study was obtained from the institutional review board of the hospital, and informed consent was obtained from all participants or their legal guardians. The collected data were analyzed to evaluate the efficacy of the comprehensive management strategies employed and their impact on patient outcomes.
3. Results
|
Variable |
n (%) |
|
Age (years) |
|
|
18–30 |
12 (30%) |
|
31–45 |
18 (45%) |
|
46–60 |
10 (25%) |
|
Gender |
|
|
Male |
32 (80%) |
|
Female |
8 (20%) |
|
Occupation |
|
|
Agricultural Worker |
16 (40%) |
|
Construction Worker |
12 (30%) |
|
Other |
12 (30%) |
|
Injury Cause |
|
|
Road Traffic Accident |
20 (50%) |
|
Agricultural Machinery |
8 (20%) |
|
Industrial Accident |
12 (30%) |
|
Time to Hospital Admission |
|
|
<6 hours |
8 (20%) |
|
6–24 hours |
20 (50%) |
|
>24 hours |
12 (30%) |
Table 1: Demographic and Clinical Characteristics of the Study Population.
The study included 40 patients with degloving injuries complicated by jaundice and septicemia. The majority of patients (45%) were between the ages of 31 and 45 years, with 30% aged 18–30 years and 25% aged 46–60 years. Male patients accounted for 80% of the study population, while females comprised 20% (Table 1). Regarding occupational background, agricultural workers were the most represented group, accounting for 40% of patients, followed by construction workers (30%) and individuals in other occupations (30%). Road traffic accidents were the leading cause of injuries (50%), followed by industrial accidents (30%) and agricultural machinery incidents (20%). A significant proportion of patients (50%) were admitted to the hospital within 6–24 hours of injury, while 20% arrived within 6 hours, and 30% were admitted after more than 24 hours (Table 2).
|
Variable |
n (%) |
|
Location of Injury |
|
|
Lower Extremity |
25 (62.5%) |
|
Upper Extremity |
10 (25%) |
|
Multiple Sites |
5 (12.5%) |
|
Associated Vascular Compromise |
|
|
Present |
28 (70%) |
|
Absent |
12 (30%) |
|
Septicemia Severity (SOFA Score) |
|
|
Mild (1–5) |
10 (25%) |
|
Moderate (6–10) |
20 (50%) |
|
Severe (>10) |
10 (25%) |
|
Jaundice (Bilirubin Levels) |
|
|
Mild (<3 mg/dL) |
15 (37.5%) |
|
Moderate (3–5 mg/dL) |
18 (45%) |
|
Severe (>5 mg/dL) |
7 (17.5%) |
Table 2: Severity and Complications of Degloving Injuries.
The majority of degloving injuries involved the lower extremity, accounting for 62.5% of cases, while 25% affected the upper extremity and 12.5% involved multiple sites. Vascular compromise was observed in 70% of the patients, emphasizing the high risk of ischemic complications associated with these injuries (Table 3). Regarding the severity of septicemia, as assessed by the SOFA score, 50% of patients had moderate septicemia (scores 6–10), while 25% presented with mild (scores 1–5) and severe (scores >10) cases, respectively. Jaundice severity, based on bilirubin levels, revealed that 45% of patients exhibited moderate jaundice (3–5 mg/dL), followed by 37.5% with mild jaundice (<3 mg/dL) and 17.5% with severe jaundice (>5 mg/dL).
|
Management Approach |
n (%) |
|
Wound Management |
|
|
Debridement and Primary Closure |
20 (50%) |
|
Skin Grafting |
15 (37.5%) |
|
Flap Reconstruction |
5 (12.5%) |
|
Infection Control Measures |
|
|
Empirical Antibiotics |
40 (100%) |
|
Targeted Antibiotics (Culture-based) |
25 (62.5%) |
|
Sepsis Management Protocol |
30 (75%) |
|
Supportive Therapy |
|
|
Blood Transfusion |
12 (30%) |
|
Nutrition Support |
35 (87.5%) |
|
Ventilator Support |
8 (20%) |
Table 3: Management Strategies and Interventions.
The management of degloving injuries involved a combination of surgical and supportive interventions tailored to the severity and complications of each case. Wound management strategies included debridement and primary closure in 50% of patients, skin grafting in 37.5%, and flap reconstruction in 12.5%. Infection control was universally implemented, with all patients receiving empirical antibiotics, and 62.5% benefiting from targeted antibiotic therapy based on culture results. Sepsis management protocols were employed in 75% of cases to address systemic complications (Table 4). Supportive therapy was a critical component, with 87.5% of patients receiving nutritional support, 30% requiring blood transfusions, and 20% needing ventilator support.
|
Outcome Variable |
n (%) |
|
Survival Rate |
|
|
Survived |
35 (87.5%) |
|
Mortality |
5 (12.5%) |
|
Functional Recovery |
|
|
Full Recovery |
20 (50%) |
|
Partial Recovery |
15 (37.5%) |
|
Permanent Disability |
5 (12.5%) |
|
Hospital Stay Duration (Days) |
|
|
<10 |
10 (25%) |
|
10–20 |
25 (62.5%) |
|
>20 |
5 (12.5%) |
Table 4: Outcomes of Management.
The outcomes of the management strategies implemented in this study were largely favorable, with an overall survival rate of 87.5%. Among the survivors, 50% achieved full functional recovery, while 37.5% experienced partial recovery, and 12.5% sustained permanent disabilities (Table 5). The duration of hospital stay varied, with the majority of patients (62.5%) hospitalized for 10–20 days, 25% discharged within 10 days, and 12.5% requiring more than 20 days of inpatient care.
|
Variable |
Survivors (n=35) |
Deceased (n=5) |
p-value |
|
Age >45 years |
10 (28.6%) |
4 (80%) |
0.03 |
|
SOFA Score >10 |
5 (14.3%) |
5 (100%) |
<0.001 |
|
Time to Admission >24 hours |
8 (22.9%) |
4 (80%) |
0.02 |
|
Severe Jaundice (>5 mg/dL) |
2 (5.7%) |
5 (100%) |
<0.001 |
|
Multiple-site Degloving Injury |
2 (5.7%) |
3 (60%) |
0.01 |
Table 5: Factors Associated with Mortality.
Analysis of factors associated with mortality revealed significant associations with several clinical and demographic variables. Age greater than 45 years was more common among deceased patients (80%) compared to survivors (28.6%), with a statistically significant difference (p=0.03). All deceased patients had a SOFA score greater than 10, compared to 14.3% of survivors (p<0.001), highlighting the severity of septicemia as a critical risk factor. Similarly, severe jaundice (bilirubin >5 mg/dL) was present in all deceased patients but only in 5.7% of survivors (p<0.001). Time to hospital admission exceeding 24 hours was associated with significantly higher mortality (80% vs. 22.9%; p=0.02). Furthermore, multiple site degloving injuries were significantly more prevalent in deceased patients (60%) compared to survivors (5.7%; p=0.01).
4. Discussion
The present study provides a comprehensive analysis of degloving injuries complicated by jaundice and septicemia, highlighting the clinical challenges, management strategies, and outcomes observed in a resource-limited setting. The demographic profile of patients in our study, predominantly male (80%) and aged between 31–45 years (45%), aligns with findings from global trauma studies, where young males are disproportionately affected due to occupational and high-risk activities [15,16]. The predominance of agricultural workers (40%) among our cases reflects the vulnerability of individuals engaged in manual labor, a trend also reported in studies on rural and industrial injuries in low- and middle-income countries (LMICs) [9]. Road traffic accidents (RTAs), the leading cause of degloving injuries in our cohort (50%), are consistent with prior research emphasizing RTAs as a major contributor to trauma in LMICs [12]. The severity of complications observed in our study underscores the critical nature of degloving injuries. Lower extremities were the most commonly affected sites (62.5%), and 70% of cases involved vascular compromise, indicating significant ischemic risks. These findings align with studies emphasizing vascular damage as a critical complication in trauma [4,17]. The distribution of septicemia severity, with 50% of cases classified as moderate by SOFA scores, and the high prevalence of moderate (45%) and severe jaundice (17.5%), reinforce the systemic burden posed by these injuries. These observations are comparable to findings from other studies linking SOFA scores with mortality and organ dysfunction in severe infections and trauma [18,19]. Management of degloving injuries in our cohort involved a multidisciplinary approach, with debridement and primary closure being the most common wound management strategy (50%), followed by skin grafting (37.5%) and flap reconstruction (12.5%). These findings are consistent with global trends emphasizing debridement and reconstructive techniques as primary interventions for extensive tissue loss [20,21]. Antibiotic therapy was universally administered, with culture-based targeted antibiotics used in 62.5% of cases, reflecting best practices for infection control in resource-limited settings [22]. Nutritional support (87.5%), blood transfusions (30%), and ventilatory support (20%) further highlight the systemic care required for such injuries, comparable to findings in studies emphasizing holistic trauma care [23]. The overall survival rate in our study was 87.5%, with full functional recovery achieved in 50% of survivors, while 37.5% experienced partial recovery and 12.5% sustained permanent disabilities (Figure 1). These outcomes are favorable compared to mortality rates reported in studies on similar trauma cases, which often exceed 20% in severe injuries [24]. However, delayed hospital admission (>24 hours) significantly increased mortality (80% vs. 22.9%; p=0.02), emphasizing the critical importance of timely intervention, a finding corroborated by research linking delayed care to poor outcomes [25]. Similarly, age >45 years, multiple-site injuries, severe jaundice (>5 mg/dL), and SOFA scores >10 were all significantly associated with mortality, mirroring global evidence on the prognostic value of these factors in trauma and sepsis management [26,27]. The study also highlights critical gaps in trauma care infrastructure, particularly in LMICs like Bangladesh. Delayed admissions due to socio-economic barriers, lack of specialized facilities, and insufficient resources exacerbate morbidity and mortality. Addressing these systemic challenges is vital, as emphasized in comparative studies that advocate for enhanced pre-hospital care, rapid triage, and multidisciplinary trauma units [28,29]. Future research should focus on integrating advanced surgical techniques, infection control measures, and systemic therapies with contextual adaptations to resource constraints. In conclusion, our findings underscore the complex interplay of clinical severity, systemic complications, and management strategies in degloving injuries complicated by jaundice and septicemia. The results highlight the importance of early intervention, multidisciplinary care, and systemic management in improving survival and functional outcomes. Comparisons with existing literature validate the observed trends and emphasize the urgent need for healthcare system strengthening in LMICs to address these critical challenges effectively (Figure 2).
Limitations of the Study
The study was conducted in a single hospital with a small sample size. So, the results may not represent the whole community.
5. Conclusion
This study provides a comprehensive evaluation of degloving injuries complicated by jaundice and septicemia, emphasizing the demographic, clinical, and systemic factors influencing patient outcomes. Our findings demonstrate the critical importance of timely intervention, effective wound management, and systemic care in reducing mortality and improving functional recovery. The study highlights significant associations between delayed hospital admission, severe jaundice, high SOFA scores, and increased mortality, underscoring the need for targeted interventions and robust healthcare infrastructure. Addressing these challenges in resource-limited settings, such as Bangladesh, requires context-specific strategies integrating advanced medical care and systemic support. Future research should focus on developing standardized protocols tailored to resource-constrained environments to improve survival and long-term outcomes for patients with these complex injuries.
Funding: No funding sources
Conflict of interest: None declared
Ethical approval: The study was approved by the Institutional Ethics Committee.
References
- Zagrocki L, Ross A, Hicks A. Management of Degloving Injuries of the Lower Extremity: A Case Report of a Forklift Injury. Foot & Ankle Specialist 6 (2013): 150-3.
- Lekuya HM, Alenyo R, Kajja I, et al. Degloving injuries with versus without underlying fracture in a sub-Saharan African tertiary hospital: a prospective observational study. Journal of Orthopaedic Surgery and Research 13 (2018): 2.
- Chowdhury MSH, Karim MN, Rahman MR, et al. An epidemiological study of injury in a rural community in Bangladesh. Bangladesh Medical Research Council Bulletin 41 (2015): 46-51.
- Scali ST, Lala S, Giles KA, et al. Contemporary management and outcomes of complex vascular surgical groin wound infections. Journal of Vascular Surgery 73 (2021): 1031-1040.e4.
- Pagliano P, Spera AM, Ascione T, et al. Infections causing stroke or stroke-like syndromes. Infection 48 (2020): 323-32.
- Bennett KM, Kent KC, Schumacher J, et al. Targeting the most important complications in vascular surgery. Journal of Vascular Surgery 65 (2017): 793-803.
- Rahman A, Ahmed S, Sultana R, et al. Epidemiology of Spinal Cord Injury in Bangladesh: A Five Year Observation from a Rehabilitation Center. J Spine 06 (2017).
- Tune SNBK, Mehmood A, Naher N, et al. A qualitative exploration of the facility-based trauma care for Road Traffic Crash patients in Bangladesh: When only numbers do not tell the whole story. BMJ Open 13 (2023): e072850.
- Biswas SN, Hussain RF, Happy TA, et al. Pattern of Injuries, Its Consequences and Concepts of Injury Prevention in a Rural Community in Bangladesh. KYAMC Journal 11 (2020): 118-23.
- Parvez MS, Shahriar MM. Agricultural Farm-Related Injuries in Bangladesh and Convenient Design of Working Hand Tools. Journal of Healthcare Engineering 2018 (2018): 4273616.
- Mashreky SR, Rahman A, Khan TF, et al. Hospital burden of road traffic injury: Major concern in primary and secondary level hospitals in Bangladesh. Public Health 124 (2010): 185-9.
- Ul Baset MK, Rahman A, Alonge O, et al. Pattern of Road Traffic Injuries in Rural Bangladesh: Burden Estimates and Risk Factors. International Journal of Environmental Research and Public Health 14 (2017): 1354.
- Saha PK, Rahman MM, Chowdhury MSA, et al. Traumatic Degloving Injury of Penis And Scrotum: A Case Report. Bangladesh Journal of Urology 15 (2012): 21-2.
- Antoniou D, Kyriakidis A, Zaharopoulos A, et al. Degloving Injury. Eur J Trauma 31 (2005): 593-6.
- Chelly H, Bahloul M, Ammar R, et al. Clinical characteristics and prognosis of traumatic head injury following road traffic accidents admitted in ICU “analysis of 694 cases. Eur J Trauma Emerg Surg 45 (2019): 245-53.
- Ghaffari-Fam S, Sarbazi E, Daemi A, et al. The Epidemilogical Characteristics of Motorcyclists Associated Injuries in Road Traffics Accidents; A Hospital-Based Study. Bull Emerg Trauma 4 (2016): 223-9.
- Sakai G, Suzuki T, Hishikawa T, et al. Primary reattachment of avulsed skin flaps with negative pressure wound therapy in degloving injuries of the lower extremity. Injury 48 (2017): 137-41.
- Dübendorfer C, Billeter AT, Seifert B, et al. Serial lactate and admission SOFA scores in trauma: an analysis of predictive value in 724 patients with and without traumatic brain injury. Eur J Trauma Emerg Surg 39 (2013): 25-34.
- Rodrigues-Filho EM, Fernandes R, Garcez A. SOFA in the first 24 hours as an outcome predictor of acute liver failure. Revista Brasileira de Terapia Intensiva 30 (2018): 64-70.
- Dini M, Quercioli F, Mori A, et al. Vacuum-assisted closure, dermal regeneration template and degloved cryopreserved skin as useful tools in subtotal degloving of the lower limb. Injury 43 (2012): 957-9.
- Graham GP, Helmer SD, Haan JM, et al. The use of Integra® Dermal Regeneration Template in the reconstruction of traumatic degloving injuries. J Burn Care Res 34 (2013): 261-6.
- Yuan K, Zhao B, Cooper T, et al. The management of degloving injuries of the limb with full thickness skin grafting using vacuum sealing drainage or traditional compression dressing: A comparative cohort study. Journal of Orthopaedic Science 24 (2019): 881-7.
- Han HS, Park CM, Lee DS, et al. Evaluating mortality and recovery of extreme hyperbilirubinemia in critically ill patients by phasing the peak bilirubin level: A retrospective cohort study. PLOS ONE 16 (2021): e0255230.
- Theocharidou E, Pieri G, Mohammad AO, et al. The Royal Free Hospital Score: A Calibrated Prognostic Model for Patients with Cirrhosis Admitted to Intensive Care Unit. Comparison with Current Models and CLIF-SOFA Score. Official Journal of the American College of Gastroenterology | ACG 109 (2014): 554.
- Gaini S, Relster MM, Pedersen C, et al. Prediction of 28-days mortality with sequential organ failure assessment (SOFA), quick SOFA (qSOFA) and systemic inflammatory response syndrome (SIRS) — A retrospective study of medical patients with acute infectious disease. International Journal of Infectious Diseases 78 (2019): 1-7.
- Rahmatinejad Z, Reihani H, Tohidinezhad F, et al. Predictive performance of the SOFA and mSOFA scoring systems for predicting in-hospital mortality in the emergency department. The American Journal of Emergency Medicine 37 (2019): 1237-41.
- Miao H, Liang H, Ma Y, et al. Total SOFA and SOFA Kidney are Associated with Short Term and Long term Outcoming of Sepsis-Associated Liver Injury [Internet]. Research Square (2021) [cited 2024 Nov 29].
- Nurmi I, Narinen A, Lüthje P, et al. Functional outcome and survival after hip fracture in elderly: a prospective study of 106 consecutive patients. J Orthopaed Traumatol 5 (2004): 7-14.
- Holtslag HR, Post MW, Lindeman E, et al. Long-term functional health status of severely injured patients. Injury 38 (2007): 280-9.