Silvia Mariel Ferrucci1, Luisa Angileri1*, Simona Tavecchio1,2, Emilio Berti1,2, Antonina Parafioriti3, Francesca Boggio4, Vinicio Boneschi1
1Dermatology Unit, IRCCS, Foundation Cà Granda Ospedale Maggiore Policlinico, Milan, Italy
2Dermatology Unit, Department of Pathophysiology and Transplantation, IRCCS, Foundation Cà Granda Ospedale Maggiore Policlinico, University of Milan, Milan, Italy
3Pathology Unit, ASST Gaetano Pini, Centro Specialistico Ortopedico Traumatologico, Gaetano Pini-CTO, Milano, Italy
4Division of Pathology, IRCCS Foundation Cà Granda Ospedale Maggiore Policlinico, Milan, Italy
*Corresponding author: Angileri Luisa, Dermatology Unit, IRCCS, Foundation Cà Granda Ospedale Maggiore Policlinico, Milan, Italy.
Received: 26 October 2021; Accepted: 11 March 2022; Published: 31 March 2022
Introduction: Lipomatous Metaplasia (LM) is a well-known aspect associated to a variety of inflammatory and neoplastic processes.
Case presentation: Here, we describe a case of LM arising in a woman during dupilumab treatment. To our knowledge there are no data in the literature about side effects similar to the clinical picture we observed in our patient.
Conclusion: We have supposed that inhibition of IL-4, together with chronic photo-exposure, could have induced the development of mature fatty tissue in the context of a cytokine pattern modified by therapy with dupilumab.
Adipocytes; Dermis; Dupilumab; Lipomatous metaplasia; Skin discoloration
1. Case Report
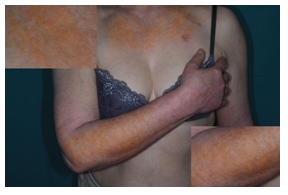
A 57-year-old woman was admitted to our Dermatology department with a severe form of early onset persistent Atopic Dermatitis (AD), phenotype generalized lichenoid with intense itch. The patient has been suffering from AD since the first months of life, with associated mild respiratory allergy. Previously she was treated with cycles of systemic steroid and phototherapy; she was unresponsive to cyclosporine and intolerant to methotrexate. She has frequently applied topical corticosteroids. The patient's quality of life was significantly deteriorated so far. In June 2019 she started therapy with dupilumab, a fully human monoclonal antibody targeting the Interleukin (IL)-4 receptor subunit α (IL-4 Rα), the common subunit of the type 2 cytokines IL-4 and IL-13, so inhibiting the entire Th2 pathway [1]. Rapidly there was a clear improvement of the AD and regression of itching and sleep disturbance; these results were further improved with good clinical remission after 12 months of therapy. The dermatitis almost cleared and the quality of life greatly improved. One year after the dupilumab therapy started, an asymptomatic yellow-orange skin discoloration appeared in areas of chronic photo-exposure such as the extensor surface of the upper limbs, the neckline, the face, and the neck; locally the skin was slightly orange-peel raised (shown in Figure 1).
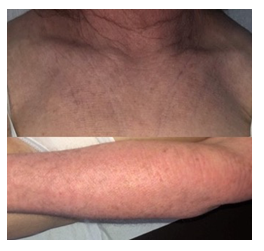
No similar cutaneous lesions were present before dupilumab treatment (shown in Figure 2).
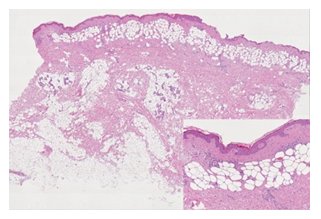
A 4 mm skin punch-biopsy was performed at the neckline and histological examination showed the presence of well vascularized adipose tissue arranged in band in the upper part of the dermis with involvement of pilosebaceous and eccrine structures; adipocytes had a mature appearance without atypical or spindle-shaped elements; the deep dermis and hypodermis were normal (shown in Figure 3).
Immunohistochemical investigations showed the fat positivity to S-100 protein, preservation of nuclear retinoblastoma immunoreactivity and negativity to MDM2, thus demonstrating a mature fat, allowing the diagnosis of Lipomatous Metaplasia (LM). Patient’s endocrine and lipid patterns were normal; ultrasonography and CT scan demonstrated no abnormal fat deposition at deep sites. The LM stabilized over the following weeks without involvement of other sites. The patient had continued the therapy with dupilumab under strict observance in order to evaluate whether it could possibly evolve or not toward a neoplastic form. In the therapy of moderate/severe AD dupilumab has always shown excellent clinical response, safety, and manageability [2, 3]. To our knowledge there are no data in the literature about side effects similar to the clinical picture we observed in our patient.
2. Discussion
LM is a well-known aspect associated to a variety of inflammatory and neoplastic processes such as scar in the ischemic heart left ventricle, gastric ulcer, neoplasia of various glands, meningioma. Moreover, it was found associated to epithelial and adnexal skin tumors [4]. In 2008 Eyerich et al [5] reported a case of cutaneous LM in a woman suffering from psoriasis vulgaris for 50 years; LM arised after two episodes of acute generalized exanthematous pustulosis, with yellow-brownish plaques localized to the thighs and upper limbs; the Authors hypothesized a relationship with the long-term skin inflammation due to psoriasis. In our patient, the cytokine pattern due to dupilumab might have been changed from type two to type one/three inflammation like that present in psoriasis, making the situation similar to the case reported by Eyerich. Indeed, Ferrucci et al [6] have reported the occurrence of psoriasis in AD patients treated by dupilumab. The presence of dermal stem cells from which mature adipocytes can derive has been demonstrated. As interleukin 4 is implicated in the dysmetabolic syndrome and seems to have a braking action on adipogenesis [7, 8], its inhibition, together with chronic photo-exposure, could have induced the development of mature fatty tissue in the context of a cytokine pattern modified by therapy with dupilumab.
Statement of Ethics
The authors have no ethical conflicts to disclose. Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Disclosure Statement
Authors declare no conflicts of interest.
Fundings
The authors received no financial support for the research, authorship, and/or publication of this article.
Author contributions
All authors contributed equally to the drafting and realization of the manuscript.
Data availability Statement
All data generated or analyzed during this study are included in this article [and/or] its supplementary material files. Further enquiries can be directed to the corresponding author.
References
- Guttman-Yassky E, Bissonnette R, Ungar B, et al. Dupilumab progressively improves systemic and cutaneous abnormalities in patients with atopic dermatitis. J Allergy Clin Immunol 143 (2019): 155-172.
- Fargnoli MC, Esposito M, Ferrucci S, et al. Real-life experience on effectiveness and safety of dupilumab in adult patients with moderate-to-severe atopic dermatitis. J Dermatolog Treat 28 (2019): 507-513.
- Nettis E, Ferrucci SM, Ortoncelli M, et al. Use of Dupilumab for 543 adult patients with moderate to severe Atopic Dermatitis: a multicenter, retrospective study. J Invest Allergol Clin Immunol (2020).
- Googe PB, Tidwell WJ, Rosenberg AE. Lipomatous metaplasia of superficial dermis. J Cutan Pathol 43 (2016): 120-124.
- Eyerich K, Traidl-Hoffmann C, Albert A, et al. Lipomatous metaplasia after severe and chronic cutaneous inflammation. Dermatology 217 (2008): 52-55.
- Ferrucci S, Tavecchio S, Berti E, et al. Acute onset of psoriasis in a patient with atopic dermatitis treated with dupilumab. Clin Exp Dermatol 45 (2020): 625-626.
- Tsao CH, Shiau MY, Chuang PH, et al. Interleukin-4 regulates lipid metabolism by inhibiting adipogenesis and promoting lipolysis. Journal of Lipid Research 55 (2014): 385-397.
- Shiau MY, Chuang PH, Yang CP, et al. Mechanism of interleukin-4 reducing lipid deposit by regulating hormone-sensitive lipase. Scientific Reports 9 (2019): 11974.