Abhishek Gaikwad, Yasmin Khan
Metro hospital and cancer research centre, Jabalpur, India
*Corresponding author: Abhishek Gaikwad, Metro hospital and cancer research centre, Jabalpur, India
Received: 15 September 2019; Accepted: 19 September 2019; Published: 23 September 2019
Background: Cardiovascular diseases are rapidly emerging as major cause of mortality and disability in India. Existing Risk Calculators for Cardiovascular Risk have not undergone appropriate validation in Indian Patients. Present Study was undertaken to compare different cardiovascular calculators for CVD risk assessment models in Indian patients presenting with first episode of myocardial infarction.
Methods: This study included 150 patients presenting with first episode of myocardial infarction (MI). 10-year risk of CVD was calculated using three risk assessment models Framingham Risk score (Risk FRS), Revised American College of Cardiology/American Heart Association (Risk ACC/AHA) and WHO Risk Prediction Charts.
Results: Risk FRS recognized the highest number of patients (74%) at high CVD risk (>20% 10 yr CV Risk) while Risk ACC/AHA and WHO ISH Risk calculators provided inferior risk discrimination. Risk FRS and Risk ACC/AHA had good correlation (Pearson's r 0.93, p<0.001) but poor agreement when divided into Subcategories (Kappa =0.022).
Conclusion: FRS seems to be as most useful CVD risk assessment tool in identification of Indian patients at high Cardiovascular Risk.
Cardiovascular Risk; Myocardial infarction
Introduction
India is in the throes of a Cardiovascular epidemic. South Asians have been seen to have higher risk of CV disease as compared to other populations [1-7]. Several Studies have shown that Cardiovascular risk among Indians is several times higher than in other ethnic groups and at least four times that of Caucasians [8,9]. Indians tend to develop CVD at a younger age (approximately 10 years) compared to others [5,6]. Both the genetic make-up and the early onset of conventional CV risk factors are believed to contribute to this excess risk [4,6].
Given the high prevalence of Cardiovascular Risk Factors in India, risk prediction models are ideal for recognizing and treating high-risk populations [10]. The cardiovascular (CV) risk assessment is carried out by determining the occurrence and severity of CV risk factors using risk calculator and prediction charts to compute overall Cardiovascular risk [11-13]. Estimation of cardiovascular risk prediction models are important in the prevention and management of CVD. Many risk estimation systems are in existence; Framingham risk score (Risk FRS), American College of Cardiology (ACC) (Risk ACC / AHA) and Joint British Societies risk calculator (Risk JBS) and WHO Risk prediction charts are commonly used [11-14].
While most of these risk estimation models have used some south Asian cohort for their derivation, None of the available risk prediction models have been prospectively validated in Indian patients. Some studies [15-18] have attempted to assess discriminating ability of CVD risk score to diagnose high risk patients (those with established Cardiovascular disease or MI) in Indian patients with conflicting results. Most of these validation studies have used older versions of AHA Risk Score, which has recently been updated [14] with new cohort data and none of these studies include comparative study of discriminaton of these Rsk scores.
Hence, the present study was to determine the comparison and validations of different 10-year CVD risk assessment models (Risk FRS, calibrated Risk ACC/AHA and Risk JBS) in Indian Cohort.
Material and Methods
Our Cohort included 150 consecutive patients admitted in coronary care unit of a tertiary Hospital between Jan 2018 to Jan 2019 with first episode of Myocardial infarction.
The diagnosis Of MI was based on 3rd universal definition of MI. All patients were admitted and managed according to current guidelines for the management of MI
History and clinical examination were done in each patent especially with respect to the presence of significant CVD risk factors.Physical examination consisted of General Physical examination and examination of Cardiovascular (CV) system. Height and body weight were measured and body mass index (BMI) was calculated. Smoking, diabetes and hypertension were defined according to the National Health Interview Survey (NHIS).
Biochemical parameters Fasting and Random blood sugar, Lipid profile was performed in every patient. Systolic and diastolic Blood pressure was recorded in each patient. Ethical clearance for the study was taken from the institutional ethical committee.
Risk Score calculation
Three risk calculators (Risk FRS, WHO ISH RISK and Risk ACC/AHA) were used to calculate 10-year risk of having a major CV event (CV death, MI or stroke) for every patent. In Risk ACC/AHA calculator, the race was taken into account as an additional factor.
Calculators were available on the following websites (https://www.framingham heartstudy.org/risk-functions/cardiovascular-disease/10-yearrisk.php#, https://sanjaybasu.shinyapps.io/ascvd/). whoshRsk R package. Was used to calculated WHO-ISH RISK. Using different risk calculators, 10-year CVD risks were divided into the five sub- categories -low risk (<10%,10-20%) and high risk (20-30%, 30-40%,>=40%) groups in each model to identify which model maximally identifies the high-risk groups. Age, gender, total and HDL cholesterol, diabetes, smoking status and treatment for hypertension were considered in FRS-CVD risk score calculation.
Statistical analysis
Statistical analysis was carried out by using R version 3.5.0. Values are expressed as mean± standard deviation or as percentages. Pearson’s correlation coefficient (r) was estimated to assess correlation between fRS and ASCVD. Kappa Score was calculated to determine agreement between various subcategories of CV Risk. Bland Altman Plot was constructed to determine bias and variation between FRS and ASCVD Risk Scores. A p-value <0.05 was considered statistically significant.
Results
Baseline Variables
Our cohort consisted of Patients who presented with first episode of MI. Some socio-demographic characteristics of our cohort was as follows :
Age: [Mean = 55.05, SD = 9.71, IQR [32.00, 78.00]. SBP: Mean = 154.27, SD = 18.96, IQR [110.00, 218.00]. DBP: Mean = 91.66, SD = 9.66,IQR [69.00, 126.00].
Around 30 % patients were Alcoholic and had a Family history of CAD, Around 40% were Diabetics. Population was predominantly Male (75.3%) and 42% were Actively Smoking.
70% cases had STEMI while 30% had NSTEMI.
Lipid Parameters were as follows :
HDL: Mean = 39.03, SD = 10.38, IQR[19.00, 74.00]. LDL: Mean = 158.55, SD = 33.01, [75.00, 242.00]. TG: Mean = 178.59, SD = 37.74,IQR [64.00, 273.00] and Total_Cholesterol: Mean = 233.31, SD = 35.06, [154.00, 318.00].
Further Details of Baseline Variables are Provided in Table 1.
|
Age |
Mean (SD) |
55.1 (9.7) |
|
Alcohol |
NO |
109 (72.7) |
|
YES |
41 (27.3) |
|
|
current_smoker |
NO |
87 (58.0) |
|
YES |
63 (42.0) |
|
|
SBP |
Mean (SD) |
154.3 (19.0) |
|
DBP |
Mean (SD) |
91.7 (9.7) |
|
Family_History |
NO |
109 (72.7) |
|
YES |
41 (27.3) |
|
|
HDL |
Mean (SD) |
39.0 (10.4) |
|
LDL |
Mean (SD) |
158.6 (33.0) |
|
TG |
Mean (SD) |
178.6 (37.7) |
|
Total_Cholesterol |
Mean (SD) |
233.3 (35.1) |
|
Sex |
FEMALE |
37 (24.7) |
|
MALE |
113 (75.3) |
|
|
MI_Type |
NSTEMI |
45 (30.0) |
|
STEMI |
105 (70.0) |
|
|
Diabetes |
NO |
90 (60.0) |
|
YES |
60 (40.0) |
|
|
Current Hypertension treatment |
NO |
91 (60.7) |
|
YES |
59 (39.3) |
|
|
Smoking |
NO |
87 (58.0) |
|
YES |
63 (42.0) |
|
|
ASCVD |
Mean (SD) |
19.7 (15.6) |
|
FRS |
Mean (SD) |
36.4 (21.6) |
Table 1: Baseline Variables
Cardiovascular Risk Scores
Framingham Risk Score (FRS),WHO ISH Risk Score (for South East Asian Region) and 10 yr ASCVD Score by new Pooled Cohort Equations were calculated.
The Scores were as Follows.
FRS: Mean = 36.42, SD = 21.63, [3.60, 90.97].
ASCVD: Mean = 19.69, SD = 15.60, [1.04, 73.57] .
A paired t test was undertaken to evaluate difference between FRS and ASCVD. The Paired t-test show that the difference between FRS and ASCVD (mean of the differences = 16.73%) was significant (t(149) = 21.99, 95% CI [15.23, 18.23], p <0.001).
Thus Framingham Risk Score more accurately identified individuals at higher risk
The Pearson's product-moment correlation between ASCVD and FRS was positive, significant and large (r = 0.93,95% C.I. 0.90-0.95 p < 0.001).
Sub-categories
The number of patients in various subcategories of 10 years risk scores were as follows:
For WHO ISH Risk Score: <10% (n = 45); 10% to <20% (n = 29);>=40% (n = 42);20% to <30% (n = 20) and 30% to <40% (n = 14).
For ASCVD Risk Score : <10% (n = 49); 10% to <20% (n = 51); 20% to <30% (n = 17); 30% to <40% (n = 12) and >=40% (n = 21).
FRS: <10% (n = 8); 10% to <20% (n = 31); 20% to <30% (n = 31); 30% to <40% (n = 26) and >=40% (n = 54).
Tabular representation in Table 2.
|
Risk Category |
FRS-Global |
AHA-ASCVD |
WHO-ISH |
|
<10% |
8 (5.3) |
49 (32.7) |
45 (30.0) |
|
10% to <20% |
31 (20.7) |
51 (34.0) |
29 (19.3) |
|
20% to <30% |
31 (20.7) |
17 (11.3) |
20 (13.3) |
|
30% to <40% |
26 (17.3) |
12 (8.0) |
14 (9.3) |
|
>=40% |
54 (36.0) |
21 (14.0) |
42 (28.0) |
Table 2: 10 years risk scores
Agreement between Scores
The agreement between ASCVD and WHO Risk Categories was Fair (weighted kappa 0.36,95% C.I. 0.18-0.55).
The agreement between FRS and WHO Risk Categories was Poor (weighted kappa 0.03,95% C.I. -0.22 - 0.27).
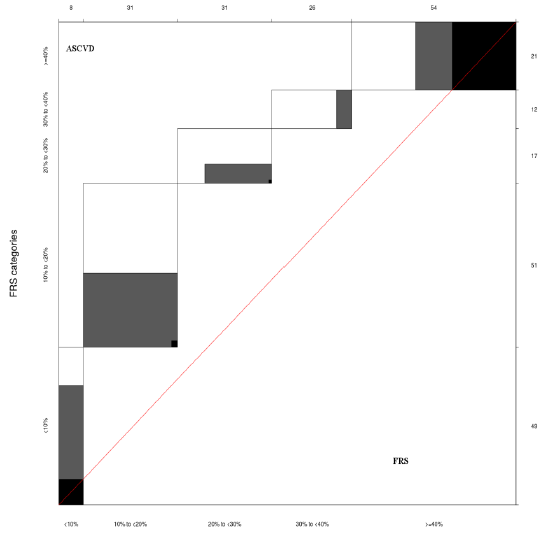
The agreement between ASCVD and FRS Categories was Poor (weighted kappa 0.022,95% C.I. -0.095 -0.14).
The agreement plot between FRS and ASCVD in Figure 1.
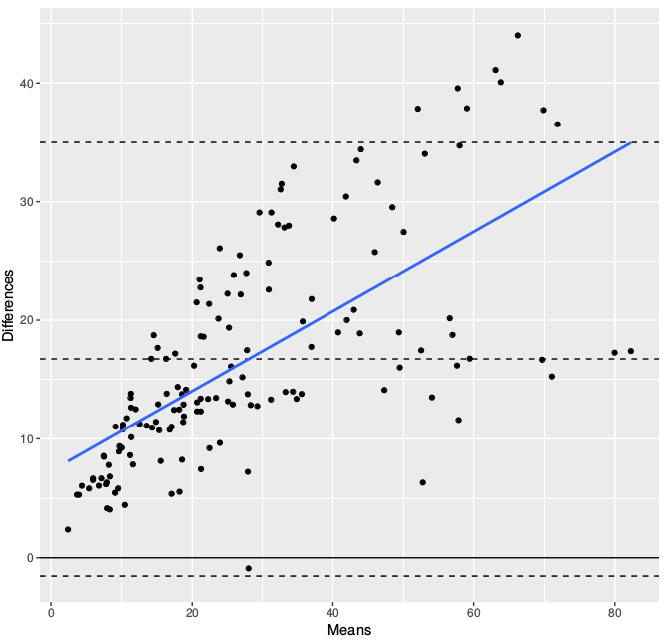
Bland Altman Analysis
Bland-Altman analysis was performed to compare FRS with ASCVD. There were 150 observations in our study. The mean risk percentage by FRS was 36.42 .The mean risk percentage by ASCVD was 19.69. There was a mean bias of 16.73 (95% C.I. 15.23 - 18.23) and 95% confidence limits of Agreement from a lower limit of -1.53 to upper limit of 35 implying 95% of differences between the two methods were found in this range. The mean proportional bias was 68.7 % with a 95% Confidence Limit of 66.21 % to 75.52 %. The difference between methods as a function of mean of two methods can be described by the equation y(differences) = 0.34 x(means) + 7.3 implying difference between two measures changes by 0.34 unit with a 1 unit increase in average of cardiovascular risk percentage calculated by two formulas. The Bland Altman Plot between FRS and ASCVD in Figure 2.
Discussion
In our study, Individuals with First episode of MI were classified as non-high risk (<20% 10 year cardiovascular Risk) in Half of Patients using ASCVD Criteria, In One -Third using WHO-ISH Risk criteria and One-Fourth Patients using Framingham Risk Score Criteria.Thus Framingham Risk Score performed best out of three scores in identifying High Risk Patients .
In Studies by Bansal et al., Garg et al and Salaam et al. [15-17] too FRS calculation yielded higher scores than WHO ISH and ASCVD Risk Scores. FRS prediction includes Cardiovascular events like myocardial infarction, Death due to a coronary event, coronary insufficiency, angina, haemorrhagic stroke, transient ischemic attack, peripheral artery disease and heart failure. In contrast WHO-ISH and ASCVD Risk Score estimate risk mainly for myocardial infarction (fatal and non- fatal) and stroke only. This can partially explain the higher individual risk per patients by FRS Score (due to broader coverage). In a Study in UK [18] it was seen that FRS calculation overestimated CV risk by approximately 5%. Bland Altman Plot also shows that overestimation rises with progressively increasing cardiovascular risk. JBS Risk Score calculation was not undertaken in our cohort.
While the correlation between FRS and AHA Risk calculator is good, agreement between their subcategories is poor which shows disadvantages of categorizing continuous data. Thus instead of using deciles of cardiovascular risk categories, absolute measures should be used and reported.
Our findings are similar to Study by Bansal and Garg where all risk Scores underestimated the 10 year Cardiovascular Risk to varying degrees. Thus we should consider looking at non-conventional measures like CIMT, hsCRP, Coronary Artery Calcium for better estimation. Our Population was slightly older to relatively younger cohort in binoo et al. (mean 36 years) but similar to Bansal and Garg et al. (mean 55-60 years) [15,16].
The strengths of our study is the use of newer AHA Pooled Cohort equation for risk estimation and analysis of evaluation of the agreement between categories of these scores by Kappa Scores and Bland Altman Plot, which has not been done previously to our knowledge in existing literature.
Our study has some limitations - These tools should ideally be measured at baseline and then cohort should be followed up in time for better assessment of risk with time. In our study we used First MI as retrospective proxy for patients with high risk. FRS-CVD is aslo not directly comparable to other tools and may not perform the best in Indians if the same outcomes were to be measured with other scores used in this study.
Conclusion
The present study shows that Most risk scores underestimated Cardiovascular Risk in India population. FRS Global Risk appeared to be most useful CVD risk assessment model in Indian patients. There was better agreement between WHO-ISH and ASCVD than with FRS,but both of them significantly underestimated cardiovascular Risk.
References
- Anand, S. S., Yusuf, S. et al. Differences in risk factors, atherosclerosis, and cardiovascular disease between ethnic groups in Canada: The Study of Health Assessment and Risk in Ethnic groups (SHARE). Lancet 356 (2000): 279–284.
- Bhopal, R., Fischbacher, C., Vartiainen, E., Unwin, N.,White, M., & Alberti, G.Predicted and observed cardiovascular disease in South Asians: Application of FINRISK, Framingham and SCORE models to Newcastle Heart Project data. Journal of Public Health 27 (2005): 93–100.
- Perumal, L., Wells, S., Ameratunga, S., Pylypchuk, R. D., Elley, C. R., Riddell, T., et al. Markedly different clustering of CVD risk factors in New Zealand Indian and European people but similar risk scores (PREDICT-14). Australian and New Zealand Journal of Public Health 36 (2012): 141–144.
- Enas, E. A., Garg, A., Davidson, M. A., Nair, V. M., Huet, B. A., & Yusuf, S.Coronary heart disease and its risk factors in ? rst-generation immigrant Asian Indians to the United States of America. Indian Heart Journal 48 (1996): 343–353.
- McKeigue, P. M., Miller, G. J., & Marmot, M. G. Coronary heart disease in South Asians overseas: A review. Journal of Clinical Epidemiology 42 (1989): 597–609.
- Joshi, P., Islam, S., Pais, P., Reddy, S., Dorairaj, P., Kazmi, K., et al . Risk factors for early myocardial infarction in South Asians compared with individuals in other countries. JAMA 297 (2007): 286-294.
- Liem SS, Oemrawsingh PV, Cannegieter SC, LeCessie S, Schreur J, et al . Cardiovascular risk in young apparently healthy descendents from Asian Indian migrants in the Netherlands: the SHIVA study. Netherlands Heart Journal 17 (2009): 155–161.
- Enas E, Senthilkumar A. Coronary artery disease in Asian Indians: An update and review. The Internet Journal of Cardiology 1 (2001): 1–22.
- McKeigue PM, Shah B, Marmot MG. Relation of central obesity and insulin resistance with high diabetes prevalence and cardiovascular risk in South Asians. Lancet 337 (1991): 382–386.
- D'Agostino RB, Sr., Pencina MJ, Massaro JM,Coady S. Cardiovascular Disease Risk Assessment: Insights from Framingham. Glob Heart 8 (2013): 11-23.
- Goff DC, Lloyd-Jones DM, Bennett G, Coady S, D’agostino RB, Gibbons R, et al. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 63 (2014): 2935-2959.
- Board JB. Joint British Societies’ consensus recommendations for the prevention of cardiovascular disease (JBS3). Heart 100 (2014): ii1-ii67.
- Mendis S, Lindholm LH, Mancia G, Whitworth J, Alderman M, Lim S, Heagerty T. World Health Organization (WHO) and International Society of Hypertension (ISH) risk prediction charts: assessment of cardiovascular risk for prevention and control of cardiovascular disease in low and middle-income countries. Journal of hypertension 25 (2007): 1578-1582.
- Yadlowsky S, Hayward RA, Sussman JB, McClelland RL, Min YI, Basu S. Clinical implications of revised pooled cohort equations for estimating atherosclerotic cardiovascular disease risk. Ann Intern Med 169 (2018): 20.
- Garg N, Muduli SK, Kapoor A, Tewari S, Kumar S, Khanna R, et al. Comparison of different cardiovascular risk score calculators for cardiovascular risk prediction and guideline recommended statin uses. Indian Heart J 69 (2017): 458-463.
- Bansal M, Kasliwal RR, Trehan N. Comparative accuracy of different risk scores in assessing cardiovascular risk in Indians: a study in patients with first myocardial infarction. Indian Heart J 66 (2014): 580-586.
- Salam AA et al. Clinical comparison of different cardiovascular risk scores for cardiovascular risk prediction in Indian patients. Int J Res Med Sci 7 (2019): 2770-2774.
- Collins GS, Altman DG. An independent and external validation of QRISK2 cardiovascular disease risk score: a prospective open cohort study. Bmj 340 (2010): c2442.