Kelly Lam1 and Devendra K. Agrawall*
1Department of Translational Research, College of Osteopathic Medicine of the Pacific, Western University of Health Sciences, Pomona, California 91766 USA.
*Corresponding author: Devendra K. Agrawal, MSc, Ph.D. (Biochem), Ph.D. (Med Sci), MBA, MS (ITM), FAAAAI, FAHA, FAPS, FIACS Professor and Director, Department of Translational Research Western University of Health Sciences 309 E. Second Street Pomona, California 91766-1854, USA
Received: 21 January 2025; Accepted: 27 January 2025; Published: 30 January 2025
Atopic dermatitis (AD), also known as eczema, is an inflammatory dermatologic condition that results in inflamed, itchy skin lesions. The development of this condition is governed by a variety of genetic and environmental factors including lifestyle habits. The severity of atopic dermatitis has been attributed to be affected by various lifestyle factors, prompting the interest in utilizing lifestyle modifications as a form of treatment for atopic dermatitis symptoms. Many research studies have been conducted to investigate the effects of different factors such as sleep, stress, diet, smoking and tobacco use, exposure to various temperatures and humidity levels, and skincare and cosmetic products on atopic dermatitis symptoms, and how certain habits can be modified to manage AD conditions. Current studies have demonstrated the significant impact some lifestyle modifications can elicit with improving atopic dermatitis, while also discussing other lifestyle factors that require further research to determine their effects on AD. This review article summarizes the findings in the current literature that investigates the role of different lifestyle habits on the severity and exacerbation of atopic dermatitis, and explores the mechanisms in which these behaviors can trigger AD.
Atopic dermatitis; Eczema; Inflammation; Lifestyle factors; Proinflammatory cytokines; Pruritus; Skin barrier
Introduction
Atopic dermatitis (AD) is a chronic inflammatory dermatologic disorder negatively impacting up to 2.6% of the global population [1]. Also known as ‘eczema,’ atopic dermatitis is generally characterized by recurring erythematous, pruritus, lichenified lesions [2]. The clinical presentation of atopic dermatitis varies depending on the severity of the condition. In more mild cases, AD presents with indistinct erythema, slightly raised epidermis, superficial excoriations, and faint lichenification [3]. Moderate cases of AD present with more visible erythema, noticeable edema, deeper excoriations, and obvious lichenification with markings [3]. In severe AD, erythema is deep and dark, visible plaques and raised papules are present and are accompanied with deep and dense excoriations [3]. Lichenification in severe AD is thick with deep markings [3]. When assessing the clinical manifestations of AD, it is important to consider the presentation variations found in lighter and darker pigmented skin.
The development of atopic dermatitis is governed by a variety of factors including associations between genetic and environmental components [4]. Additionally, there are ethnic and racial disparities in the clinical manifestations of atopic dermatitis [5]. Mutations in the filaggrin gene have a strong correlation in contributing to the susceptibility of developing atopic dermatitis [6]. The filaggrin gene is specifically responsible for the keratinization of skin, and impairment in this process results in skin barrier dysfunction [7]. Part of a complex of genes known as the epidermal differentiation complex which encodes proteins responsible for the development of the epidermal structure and barrier, studies have found that mutations in the filaggrin gene are present in roughly 25-50% of patients with AD [4-9].
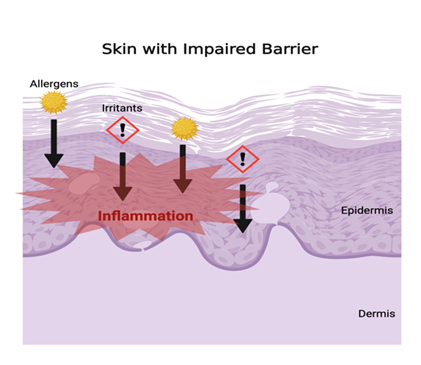
Various environmental factors also contribute to atopic dermatitis. As a result of impaired skin barrier, allergens and irritants have increased permeability and elicit greater epidermal inflammatory responses in patients with AD [10]. Common environmental factors that play a role in eliciting exacerbation of AD symptoms include air pollutants, environmental and dietary allergens, seasonal changes, temperature variation, and microbes [11, 12, 13].
There are many complications associated with atopic dermatitis including increased risk of infection and significant impacts on quality of life. Patients with AD are found to have greater prevalence of the S. Aureus bacteria which can lead to bacterial epidermal infections with common infections including impetigo, cellulitis, and abscesses [14]. Atopic dermatitis also leads to greater risk of developing viral infections such as eczema herpeticum [14]. Negative impacts to quality of life are a more common complication associated with atopic dermatitis. Common complications include severe pruritus leading to sleep deficits with other impacts to quality of life including psychosocial and mental health impacts [15].
While atopic dermatitis primarily affects the epithelial system, there are correlations between AD and morbidities with other systems of the body. Comorbidities associated with atopic dermatitis may arise due to related pathogenesis to AD or due to the effects of AD symptoms [16]. In this review, the relation between AD and other systems will be highlighted as the impact of lifestyle and modifiable factors on the manifestation of atopic dermatitis is explored.
Lifestyle and Health
Lifestyle choices are one of the most important and arguably most governable factors that can influence one’s health. Throughout the years, many research studies have been conducted analyzing the effects of daily lifestyle habits regarding topics such as sleep, stress, and diet on maintaining general health. It has been found that patients with chronic illnesses and multimorbidities are more likely to be associated with a poorer lifestyle with habits such as poor sleep hygiene, poor stress management, physical inactivity, inappropriate diet and smoking [17, 18]. To address the correlation between poor lifestyle habits and poorer health, lifestyle medicine and altering lifestyle habits can be assessed.
Lifestyle medicine is a branch of medicine that focuses on preventing and managing disease symptoms through six pillars of beliefs: plant-based diet, appropriate physical exercise, appropriate sleep hygiene, stress management, avoidance of risky substances, and maintaining positive social connections [19]. By altering one’s lifestyle to include healthier habits, studies have shown that incorporation of lifestyle medicine ideals and lifestyle modifications can offer effective improvement and management of symptoms for patients suffering from chronic diseases [20]. For patients suffering from atopic dermatitis, lifestyle management is often analyzed as a method of treatment and relief in conjunction with conventional treatment options.
Effects of Sleep
Proper sleep hygiene is an essential factor that helps restore and maintain the health of a variety of systems throughout the body. The pruritus nature of atopic dermatitis has been noted as a common cause for insomnia in patients and the development of worsened sleep quality have been shown to result in heightened atopic dermatitis conditions [21,22]. For individuals suffering from atopic dermatitis, a disturbance in sleep can cause a variety of physiological responses involving the immune system, thermoregulation of body temperature, and fluid balance that results in a flare up of AD symptoms [21,22].
One way in which sleep disorders have been found to cause atopic dermatitis flare ups is highlighted in the relation of sleep with the immune system. Studies have shown that a loss of sleep leads to a decreased release of natural killer cells and results in the skin to be more susceptible to infections. [21, 23]. A greater increase in the release of inflammatory cytokines also occurs due to loss of sleep which contributes to damaging of the skin barrier [21, 24]. Elevated cytokine levels lead to an increase in the pruritus nature of AD and coupled with the decrease of Prostaglandin E2 which assist in repairing the skin barrier and are released during sleep, further compromises skin barrier and ability for barrier damages to heal [21, 22, 25].
In relation to the immune system, another physiological response that is impacted by sleep is thermoregulation. During sleep, studies have shown that while there are variations in body temperature throughout the night, the general trend of the body’s core temperature is at its lowest during the evening [21, 26]. As sympathetic tone is decreased during sleep, vascular flow increases within the cutaneous layer resulting in heat dissipation through the skin and elevated cutaneous temperature [26, 27]. This increase in the temperature of the skin has been associated with magnified nocturnal pruritus and exacerbation of atopic dermatitis conditions [26].
During night time, the skin barrier is further compromised as a rise in transepidermal water loss (TEWL) is noted [26]. Not only has TEWL been found to naturally rise during the evening, but studies have shown that TEWL rates are even further increased in patients with AD and in individuals who have poorer sleep quality which patients with AD often report [28, 29]. Associated with TEWL increase, this physiological mechanism results in greater itch and decreased ability for repair to skin damage [28, 29].
Effects of Stress
Stress is a major factor that has significant effects on the symptoms and manifestations of atopic dermatitis. Studies have shown that different types of stress including oxidative and psychological stress can play a role in both manifestation of atopic dermatitis and the triggering of AD symptoms [30].
Oxidative stress is defined as an imbalance between oxidants and antioxidants within the body where an inclination towards oxidant levels is present [31, 32]. Increase in reactive oxygen and nitrogen species coupled with a decrease in antioxidant defense results from a variety of factors including environmental factors, psychological factors, and from the effects of aging and disease. [32-35]. Oxidative stress poses negative effects to bodily functions by increasing proinflammatory cytokines [32, 33]. In relation to cutaneous effects, an increase in proinflammatory cytokines creating an inflammatory environment can lead to the development and worsening of atopic dermatitis through increased pruritus and delayed wound healing [32, 33]. In fact in patients with AD, oxidative stress levels have been found to be markedly increased [32, 36]. A study researching the relation between oxidative stress and chronic skin conditions has discovered biomarkers of oxidative stress to be significantly elevated in the urine of patients presenting with AD, with levels of magnitude mirroring the severity of presenting symptoms [32, 36].
Psychological stress has also been indicated as a significant contributor to AD with various types of psychological stress contributing to the manifestation of eczema symptoms [33, 37]. While the mechanism of how psychological stress impacts the nature of AD is not well known, studies have indicated the state of psychological stress causes prolonged activation of the hypothalamus-pituitary-adrenal axis resulting in markedly increased release of stress biomarkers, leading to decreased immunity, delayed wound-healing, and increased TEWL in AD patients [33, 38]. In patients with AD, studies have shown AD can conversely cause worsened psychological stress and decreased quality of life due to intense pruritus, poor body image, and decreased self-confidence [33, 37-40]. While there is significant correlation between AD and psychological stress, whether the manifestations of AD precede psychiatric conditions or psychiatric conditions precede the development of eczema is still relatively unclear [37].
Effects of Diet
The link between diet and atopic dermatitis is another lifestyle factor that has been studied to better understand the association between dietary consumption and the triggering and manifestation of AD. In relation to atopic dermatitis specifically, common food allergens such as dairy, peanuts, eggs, and gluten have been associated with being common triggers for food triggered AD [41, 42]. Food triggered AD can manifest in immediate or latent reactions. AD symptoms that manifest immediately are often triggered by IgE mediated immune responses and results in the exacerbation of pruritus as well as flare ups of erythematous lesions [43]. In latent reactions, exacerbation of AD symptoms are delayed for hours to days after consumption of the food trigger [44].
For individuals who experience food triggered AD from dairy, peanuts, and eggs, studies have found that these individuals not only exhibit significantly higher levels of IgE antibodies overall, but also exhibit higher levels of specific IgE antibodies to proteins found in dairy, peanuts, eggs, and cat dander compared to individuals who do not present with AD [44]. Specifically for individuals who exhibit dairy allergies, a study examining the prevalence of AD in 100 individuals with cow’s milk allergy found that up to 71% were found to have coexisting atopic dermatitis reactions [44]. In individuals experiencing AD flare ups as a result of consuming gluten, a significant link between gluten intolerance and atopic dermatitis has been explored. The inability to properly absorb gluten and the result of inflammation from gluten consumption has been shown to lead to cutaneous manifestations such as AD [44,45].
The relationship between the gut microbiome and atopic dermatitis has also been investigated to further examine the association of food triggers and AD. In many studies that have been conducted, results have shown significant correlation between the diversity of an individual’s gut microbiome with their tendency to develop eczematous lesions [45-48]. These studies suggest that with a decreased diversity of gut microbiome, individuals suffer from dysfunctional immune responses increasing the susceptibility to allergic reactions such as AD [46-48]. Furthermore, this imbalance in gut microbiota leads to greater sensitivity to certain foods, increasing food intolerances which contributes to the exhibition of food triggered AD [49].
Effects of Alcohol
Alcohol has been known to cause negative influences on various bodily systems, most commonly known to pose negative effects on the liver. While not as well known, alcohol consumption has been indicated to have negative impacts to the skin and contributes to increasing the risk of the manifestations and exacerbation of various skin diseases. Alcohol has been found to influence the skin under various mechanisms which include alcohol’s effect on gut microbiota, increasing inflammation, vascular permeability, and promoting oxidative stress [50-54].
Multiple studies have shown that alcohol consumption has been linked with creating imbalanced gut microbiomes although the exact mechanism as to how this imbalance is induced is not well understood [55, 56]. The alcohol induced change in the gut microbiome has been found to negatively affect gut integrity which further results in impairment of the immune system and increased release of proinflammatory cytokines [56]. Chronic exposure to alcohol can also lead to additional tissue injury which results in greater inflammation [54, 56]. Furthermore, the metabolism of alcohol has also been shown to result in increased oxidative stress as the process of metabolizing alcohol generates reactive oxygen species [54]. The generation and release of reactive oxygen species is greatly elevated under inflammatory conditions [54]. The ability of alcohol to increase microvascular permeability further contributes to the inflammatory reaction to consuming alcohol as increases in vascular permeability leads to greater inflammation specifically in the skin [50, 53]. Analyzing the mechanisms in which alcohol affects the body, these effects mentioned have all been previously discussed to impact the triggering and manifestation of atopic dermatitis conditions.
In many analyses conducted on the relationship between alcohol and atopic dermatitis, the effect of alcohol consumption during pregnancy on the risk of the offspring developing AD is a popular topic. While it is not clear if there is a direct causation between maternal alcohol consumption and later on development of AD in their offsprings, many studies have demonstrated a correlation that indicates alcohol consumption during pregnancy as a probable risk factor to developing eczema in the child’s life. A study conducted by Linnenberg et al., had shown that the risk of atopic dermatitis development in offsprings was significantly impacted by maternal alcohol consumption and is dose dependent [57]. The results of the study showed that the greatest risk for AD development was seen when maternal alcohol consumption reached four or more drinks a week at 30 weeks gestation [57]. In a longitudinal study conducted by Carson et al., a significant association between alcohol consumption and atopic dermatitis development was demonstrated with the greatest risk of AD development to present within the first 7 years of the child’s life [58]. A study later conducted by Wada et al., further demonstrated the increased risk of atopic dermatitis where they found a positive association between maternal alcohol intake with increasing risk of atopic dermatitis within the first 5 years of life [59].
Effects of Smoking Tobacco
Smoking has been indicated in multiple studies to be a contributing factor to atopic dermatitis. Tobacco smoke has been shown to pose many negative effects to an individual’s general health with many studies demonstrating the development of immune system dysfunction and chronic inflammation as a result of cigarette use [60, 61]. The direct effects of tobacco smoke on the skin has been researched with studies indicating the elevated oxidative stress that results from smoking, and the impairment of the immune system, negatively impacts the skin’s protective barrier resulting in the development of various skin conditions [60, 62, 63, 64]. Discussing the effects of smoking on atopic dermatitis specifically, many studies have been conducted to explore the relationship between smoking and AD, with various conditions including active smoking or second hand exposure to smoke, different age ranges, and maternal exposure to smoke being analyzed.
Comparing the effects of direct smoke exposure to secondhand smoke exposure, studies have shown that both types of exposure to tobacco smoke result in a positive association with the development of AD [60]. In individuals who have direct exposure to tobacco smoke, studies have shown that there is a positive correlation in active smoking with AD development in both adults over the age of 18 and children under the age of 18 [60, 65]. Even in adults who do not exhibit a predisposition to atopic dermatitis, participating in direct smoking increases the prevalence of adult onset AD [66]. In individuals who are exposed to secondhand tobacco smoke, a positive association with AD was also found [60, 67]. However, in passive smoke exposure, studies have indicated that the risk of developing AD is greater in adults compared to children [60].
Maternal exposure to tobacco smoke and the risk of their offspring developing AD was also a popular topic that was explored. In many studies conducted, the results have shown that there is no significant association with maternal smoking and development of AD in offsprings [60]. However, other studies have produced conflicting results that have found an increase in risk of AD development in offsprings due to maternal tobacco exposure [68-70]. In some studies, it has even been found that while there was no significant association between active maternal smoking and AD risk in offsprings, a significant correlation was noted between passive maternal smoking, such as secondhand exposure, and risk of AD manifestation in offsprings [68, 71]. From these findings, it is still unclear whether there is an association between maternal exposure to tobacco smoke and development of AD in offsprings. More studies will have to be conducted to produce a more conclusive understanding of this topic.
Effects of Temperature and Humidity
Various environmental factors play a role in managing atopic dermatitis symptoms, and conflicting results have been produced demonstrating the effects of temperature and humidity in individuals with AD [72]. Looking at the studies conducted in regard to the effects of temperature on AD, some studies have found that an increase in temperature results in reduced manifestation of AD [72-74]. In a paper published by Kantor et al., the article hypothesizes the relationship between higher temperatures with greater UV exposure to be the contributing factor to improved AD, as UV has been shown to have beneficial effects for eczematous conditions [72]. One proposed mechanism in which UV is beneficial to AD is it helps produce Vitamin D which is often found to be deficient in individuals who have atopic dermatitis, with levels of deficiency correlating with the severity of AD symptoms [75-77]. Other studies and research articles have produced contradictory results that demonstrated an increase in temperature to exacerbate AD symptoms. In a paper by Sargen et al., the article states that higher temperatures promote TEWL which is a major contributing factor to AD [78]. Warmer temperatures also lead to increased sweating which was seen in a study conducted by Langan et al., to be positively correlated with eczematous flare ups in individuals with AD [79]. Sweat produces inflammatory markers that are associated with dysfunction of the filaggrin gene which is positively correlated with the clinical manifestation of AD [79, 80].
Exploring studies that relate levels of humidity with AD prevalence, contrasting results were similarly found. In some studies, it has been found that under conditions of high humidity, protective measures against atopic dermatitis have been noted as the increase in humidity reinforces the skin’s barrier [73]. When the skin is exposed to environments where there is low humidity, studies have shown this leads to increasing TEWL resulting in dysfunction of the skin barrier and eczematous conditions [73, 81]. Lower humidity also results in increased production of inflammatory markers such as Interleukin-1 alpha, and keratinocyte proliferation which further exacerbates AD symptoms [73, 82, 83, 84]. In other studies, contradicting results have been produced demonstrating that an increase in humidity exacerbates AD instead as humid environments can contribute to increased sweating [78-80].
Effects of Skincare and Cosmetic Products
There are many skincare products available that can produce beneficial results for individuals suffering from atopic dermatitis, but the ingredients in some products in the market can produce detrimental effects triggering AD flare ups and worsening AD symptoms. Two common ingredients found in skincare and cosmetic products that often induce AD symptoms include fragrance and parabens.
Fragrance is present in most skincare and cosmetic products and is often found to be a main trigger for skin reactions. The mechanism in which fragrances affect the skin is attributed to a magnified immune response [85]. In individuals more susceptible to allergies including those with atopic dermatitis, studies have shown that fragrance leads to an increase in cytokine release and increases inflammatory responses [85]. Studies have also shown that different sexes and age groups have different susceptibility patterns to fragrance triggered AD. Females have been found to be more susceptible to atopic dermatitis reactions towards fragrances compared to males which studies have hypothesized is due to the increased exposure females tend to have to products with fragrances [86-89]. Younger populations also tend to have increased exposure patterns to fragrances compared to older populations which leads to greater rates of fragrance triggered AD in the younger population [87].
Besides fragrance, the use of parabens in skincare and cosmetic products have also been shown to induce AD flare-ups. Parabens are a common preservative used to prevent the growth of bacteria and fungi that is found in most skincare and cosmetic products including makeup, body cleansing products, and even oral hygiene products [90, 91]. The mechanism in how parabens trigger AD is still not well known, though studies have shown that parabens act as endocrine disrupting compounds and can modulate the immune system through modifying cytokine and IgE production [92, 93]. Similarly to fragrance, the effects of parabens on the susceptibility of AD vary depending on age ranges. In many studies, it has been shown that paraben exposure during early childhood and prenatal exposure leads to greater risk for AD development, specifically early-onset atopic dermatitis, due to exposure during the maturation of the immune system [94-96]. Different from the effects of fragrance, studies have shown conflicting results regarding the effects of parabens on AD prevalence among different sexes. In a study conducted by Vindenes et al., females have demonstrated to possess higher levels of parabens in their urine due to greater exposure to personal care products, leading to greater susceptibility to paraben triggered AD [97]. In contrast, in a study conducted by Arafune et al., despite different exposure patterns to paraben-containing products that are observed between females and males, no significant difference was observed in the effect of parabens on AD [95].
Preventive Lifestyle Modifications for Atopic Dermatitis
Analyzing the effects of different lifestyle factors that can impact atopic dermatitis, many studies have explored lifestyle modifications that can be utilized to manage AD symptoms. In response to the effects of stress on AD, participating in de-stressing activities such as listening to music, breathing exercises, physical activity, and meditation have been shown to significantly reduce stress, anxiety, and depression which can manage the effect of stress on AD [98, 99]. Diet modifications can also be made in order to manage AD symptoms. In a study conducted by Dhar et al., out of 100 individuals tested, significant improvement in AD was observed when certain foods including dairy, peanuts, eggs, seafood, and beans were eliminated from their diet for 3 weeks [100]. Other studies have also suggested significant improvement in AD symptoms through limiting the consumption of sweets [43, 101]. As alcohol consumption and tobacco use have both been associated with increasing the severity of AD, cessation of these activities may result in improvement of AD [66, 102]. In terms of temperature and humidity effects on AD, there is still much debate regarding which climatic factors are more beneficial for symptom management so it is unclear whether avoiding one climate over the other would prove to be a significant modification for AD management. Skincare and cosmetic modifications that can be implemented include avoiding products that contain fragrances and parabens, and to incorporate products that contain antioxidants and anti-inflammatory properties [103]. Products that include prebiotics have also been shown to improve AD symptoms and reduce pruritus through restoring the skin microbiome and barrier [104]. Topical pharmaceutical creams and treatments can also be utilized to manage AD flare-ups with common options including corticosteroids, non-steroidal agents, anti-inflammatory drugs, and calcineurin inhibitors [105-107]. Through practicing modifications and utilizing treatments to reduce the symptoms of AD, sleep hygiene can also be improved. Through improving sleep, studies have shown greater restoration to the skin barrier and improvement to AD conditions [108, 109].
Conclusion
The research shows that lifestyle factors can play a significant role in the clinical manifestation and triggering of atopic dermatitis symptoms. The literature shows lack of sleep, psychological and oxidative stress, and certain foods including dairy, eggs, peanuts, and gluten, can all contribute to the exacerbation of AD. Alcohol use and tobacco use both contribute to worsening AD, and in cases where maternal smoking and alcohol consumption is occurring, the risk of AD development in offsprings can be increased. The effects of temperature and humidity on atopic dermatitis is still unclear with studies producing contradictory results in regard to which conditions provide beneficial or detrimental effects to individuals diagnosed with AD. Personal care products containing fragrances and parabens can also worsen atopic dermatitis. Studies have shown that due to variations in exposure, females and younger populations tend to be more susceptible to fragrance triggered AD. Younger populations also tend to be more susceptible to paraben triggered AD compared to older populations. Overall, these findings implicate the importance of considering lifestyle factors when assessing and treating atopic dermatitis. Along with other treatments available, lifestyle modifications can serve to be significant treatment options, and can play a contributory role to improving the quality of life of individuals with atopic dermatitis.
Major Key Points and Outstanding Questions
- • Lifestyle habits promoting inflammation are strong triggers for atopic dermatitis.
- • Lifestyle modifications that protect and restore the skin barrier are important in preventing the manifestation of atopic dermatitis.
- • Lifestyle changes that promote overall health are beneficial for managing eczema.
- • How attainable is using lifestyle modifications to manage atopic dermatitis for individuals of low socioeconomic backgrounds?
- • Is the usage of lifestyle modifications alone without traditional eczema treatments enough to provide significant long-term improvement to atopic dermatitis?
- • How do certain genetic factors impact the effects of lifestyle factors and modifications on atopic dermatitis?
- • What benefits are there to using lifestyle modifications over traditional eczema treatments?
- • What differences causes the stark variations in how temperatures and humidity levels affect the atopic dermatitis conditions of different individuals?
Funding:
The research work of DKA is supported by the R25AI179582 and R01 HL147662 grants from the National Institutes of Health, USA. The contents of this article are solely the responsibility of the authors and do not necessarily represent the official views of the National Institutes of Health.
Competing interests:
Both authors have read the manuscript and declare no conflict of interest. No writing assistance was utilized in the production of this manuscript.
Consent for publication:
Both authors have read the manuscript and consented for publication.
References
- Tian J, Zhang D, Yang Y, et al. Global epidemiology of atopic dermatitis: a comprehensive systematic analysis and modelling study. British Journal of Dermatology 190 (2024): 55-61.
- Frazier W, Bhardwaj N. Atopic Dermatitis: Diagnosis and Treatment. American Family Physician. Published May 15 (2020): 590-598.
- Hanifin J, Baghoomian W, Grinich E, et al. The Eczema Area and Severity Index - A Practical Guide. Dermatitis 33 (2022): 187-192.
- Chaudhary F, Lee W, Escandar T, et al. Exploring the Complexities of Atopic Dermatitis: Pathophysiological Mechanisms and Therapeutic Approaches. J Biotechnol Biomed 7 (2024): 314-328.
- Chaudhary F, Agrawal DK. Ethnic and Racial Disparities in Clinical Manifestations of Atopic Dermatitis. Arch Intern Med Res 7 (2024): 114-133.
- Gupta J, Margolis D. Filaggrin gene mutations with special reference to atopic dermatitis. Curr Treat Options Allergy 7 (2020): 403-413.
- Afshari M, Kolackova M, Rosecka M, et al. Unraveling the skin; a comprehensive review of atopic dermatitis, current understanding, and approaches. Front Immunol 15 (2024): 1361005.
- Biagini Myers J, Khurana Hershey G. Eczema in Early Life: Genetics, the Skin Barrier, and Lessons Learned from Birth Cohort Studies. The Journal of Pediatrics 157 (2010): 704-714.
- Osawa R, Akiyama M, Shimizu H. Filaggrin Gene Defects and the Risk of Developing Allergic Disorders. Allergology International 60 (2011): 1-9.
- Ricardo Criado P, Amante Miot H, Bueno-Filho R, et al. Update on the pathogenesis of atopic dermatitis. Anais Brasileiros de Dermatologia 99 (2024): 895-915.
- Luschkova D, Zeiser K, Ludwig A, et al. Atopic eczema is an environmental disease. Allergologie select 5 (2021): 244-250.
- Chong A, Visitsunthorn K, Ong P. Genetic/Environmental Contributions and Immune Dysregulation in Children with Atopic Dermatitis. Journal of Asthma and Allergy 15 (2022): 1681-1700.
- Lee W, Chaudhary F, Agrawal DK. Environmental Influences on Atopic Eczema. J Environ Sci Public Health 8 (2024): 101-115.
- Wang V, Boguniewicz J, Boguniewicz M, et al. The infectious complications of atopic dermatitis. Annals of Allergy, Asthma & Immunology 126 (2021): 3-12.
- Na C, Chung J, Simpson E. Quality of Life and Disease Impact of Atopic Dermatitis and Psoriasis on Children and Their Families. Children 6 (2019): 133.
- Silverberg J. Comorbidities and the impact of atopic dermatitis. Annals of Allergy, Asthma & Immunology 123 (2019): 144-151.
- Niebuur J, Vonk J, Du Y, et al. Lifestyle factors related to prevalent chronic disease multimorbidity: A population-based cross-sectional study. Plos One 18 (2023): e0287263.
- Oster H, Chaves I. Effects of Healthy Lifestyles on Chronic Diseases: Diet, Sleep and Exercise. Nutrients 15 (2023): 4627.
- Lippman D, Stump M, Veazey E, et al. Foundations of Lifestyle Medicine and its Evolution. Mayo Clinic Proceedings: Innovations, Quality & Outcomes 8 (2024): 97-111.
- Sadiq I. Lifestyle medicine as a modality for prevention and management of chronic diseases. Journal of Taibah University Medical Sciences 18 (2023): 1115-1117.
- Mann C, Gorai S, Staubach-Renz P, et al. Sleep disorders in dermatology - a comprehensive review. Journal der Deutschen Dermatologischen Gesellschaft 21 (2023): 577-584.
- Lavery M, Stull C, Kinney M, et al. Nocturnal Pruritus: The Battle for a Peaceful Night’s Sleep. International Journal of Molecular Sciences 17 (2016): 425.
- Zhu J, Peng K, Zhang Y, et al. Sleep quality, circadian preferences, and mood among patients with acne vulgaris: a case-control study. Sleep Breath 27 (2023): 1997-2003.
- Gamaldo C, Shaikh A, McArthur J. The Sleep-Immunity Relationship. Neurologic Clinics 30 (2012): 1313-1343.
- Cheng H, Huang H, Guo Z, et al. Role of prostaglandin E2 in tissue repair and regeneration. Theranostics 11 (2021): 8836-8854.
- Thorburn P, Riha R. Skin disorders and sleep in adults: where is the evidence? Sleep Medicine Reviews 14 (2010): 351-358.
- Szymusiak R. Body temperature and sleep. Handbook of Clinical Neurology 156 (2018): 341-351.
- Iwanaszko M, Waldeck N, Anafi R, et al. Circadian rhythms in skin barrier function in atopic dermatitis: A pilot study. Journal of Biological Rhythms 39 (2024): 208-214.
- Oyetakin-White P, Suggs A, Koo B, et al. Does poor sleep quality affect skin ageing? Clinical and Experimental Dermatology 40 (2015): 17-22.
- Alessandrello C, Sanfilippo S, Minciullo P, et al. An Overview on Atopic Dermatitis, Oxidative Stress, and Psychological Stress: Possible Role of Nutraceuticals as an Additional Therapeutic Strategy. International Journal of Molecular Sciences 25 (2024): 5020.
- Raimondo A, Serio B, Lembo S. Oxidative Stress in Atopic Dermatitis and Possible Biomarkers: Present and Future. Indian Journal of Dermatology 68 (2024): 657-660.
- Sies, H. Oxidative Stress: Concept and Some Practical Aspects. Antioxidants 9 (2020): 852.
- Bertino L, Guarneri F, Cannavò S, et al. Oxidative Stress and Atopic Dermatitis. Antioxidants 9 (2020): 196.
- Sies H, Berndt C, Jones D. Oxidative Stress. Annual Review of Biochemistry 86 (2017): 715-748.
- Liguori I, Russo G, Curcio F, et al. Oxidative stress, aging, and disease. Clinical Interventions in Aging 13 (2018): 757-772.
- Nakai K, Yoneda K, Maeda R, et al. Urinary biomarker of oxidative stress in patients with psoriasis vulgaris and atopic dermatitis. Journal of the European Academy of Dermatology and Venereology 23 (2009): 1405-1408.
- Talamonti M, Galluzzo M, Silvaggio D, et al. Quality of Life and Psychological Impact in Patients with Atopic Dermatitis. Journal of Clinical Medicine 10 (2021): 1298.
- Iannone M, Janowska A, Panduri S, et al. Impact of psychiatric comorbidities in psoriasis, hidradenitis suppurativa and atopic dermatitis: The importance of a psychodermatological approach. Experimental Dermatology 31 (2022): 956-961.
- Lonndahl L, Abdelhadi S, Holst M, et al. Psychological Stress and Atopic Dermatitis: A Focus Group Study. Annals of Dermatology 35 (2023): 342-347.
- Almutawa Y, AlGhareeb M, Bhattarai E, et al. Investigation of the Impact of Atopic Dermatitis (AD) on Stress, Depression, Anxiety, and Suicidal Ideation: A Systematic Review and Meta-Analysis. Cureus 16 (2024): e63376.
- Chang A, Robison R, Cai M, et al. Natural history of food triggered atopic dermatitis and development of immediate reactions in children. The Journal of Allergy and Clinical Immunology 4 (2016): 229-236.
- Vats V, Makineni P, Hemaida S, et al. Gluten Intolerance and Its Association With Skin Disorders: A Narrative Review. Cureus 15 (2023): e44549.
- Katta R, Schlichte M. Diet and Dermatitis: Food Triggers. Journal of Clinical and Aesthetic Dermatology 7 (2014): 30-36.
- Giannetti A, Cipriani F, Indio V, et al. Influence of Atopic Dermatitis on Cow’s Milk Allergy in Children. Medicina 55 (2019): 460.
- Shalom G, Kridin K, Raviv K, et al. Atopic Dermatitis and Celiac Disease: A Cross-Sectional Study of 116,816 Patients. American Journal of Clinical Dermatology 21 (2019): 133-138.
- Stockholm J, Blaser M, Thorsen J, et al. Maturation of the gut microbiome and risk of asthma in childhood. Nature Communications 9 (2018): 141.
- Kim J, Kim H. Microbiome of the Skin and Gut in Atopic Dermatitis (AD): Understanding the Pathophysiology and Finding Novel Management Strategies. Journal of Clinical Medicine 8 (2019): 444.
- Lopez-Santamarina A, Gonzalez E, Lamas A, et al. Probiotics as a Possible Strategy for the Prevention and Treatment of Allergies. A Narrative Review. Foods 10 (2021): 701.
- Abril A, Carrera M, Sanchez-Perez A, et al. Gut Microbiome Proteomics in Food Allergies. International Journal of Molecular Sciences 24 (2023): 2234.
- Liu L, Chen J. Advances in Relationship Between Alcohol Consumption and Skin Diseases. Clinical, Cosmetic and Investigational Dermatology 16 (2023): 3785-3791.
- Egeberg A, Weinstock L, Thyssen E, et al. Rosacea and gastrointestinal disorders: a population-based cohort study. British Journal of Dermatology 176 (2017): 100-106.
- Schopf R, Ockenfels H, Morsches B. Ethanol enhances the mitogen-driven lymphocyte proliferation in patients with psoriasis. Acta Dermato-Venereologica 76 (1996): 260-263.
- Van der Heide F, Eussen S, Houben A, et al. Alcohol consumption and microvascular dysfunction: A J-shaped association: The Maastricht Study. Cardiovascular Diabetology 22 (2023): 67.
- Jung M, Callaci J, Lying K, et al. Alcohol Exposure and Mechanisms of Tissue Injury and Repair. Alcoholism: Clinical and Experimental Research 35 (2010): 392-399.
- Pohl K, Moodley O, Dhanda A. Alcohol’s Impact on the Gut and Liver. Nutrients 13 (2021): 3170.
- Engen P, Green S, Voigt R, et al. The Gastrointestinal Microbiome. Alcohol Research Current Reviews 37 (2015): 223-236.
- Linneberg A, Petersen J, Gronbaek M, et al. Alcohol during pregnancy and atopic dermatitis in the offspring. Clinical & Experimental Allergy 34 (2004): 1678-1683.
- Carson C, Halkjaer L, Jensen S, et al. Alcohol Intake in Pregnancy Increases the Child’s Risk of Atopic Dermatitis. The COPSAC Prospective Birth Cohort Study of a High Risk Population. Plos One 7 (2012): e42710
- Wada K, Konishi K, Tamura T, et al. Alcohol Intake During Pregnancy and Offspring’s Atopic Eczema Risk. Alcoholism: Clinical and Experimental Research 40 (2016): 1037-1043.
- Kantor R, Kim A, Thyssen J, et al. Association of atopic dermatitis with smoking: A systematic review and meta-analysis. Journal of the American Academy of Dermatology 75 (2016): 1119-1125.
- Parmar M, Kaur M, Bhavanam S, et al. A Systematic Review of the Effects of Smoking on the Cardiovascular System and General Health. Cureus 15 (2023): e38073.
- Sticozzi C, Belmonte G, Pecorelli A, et al. Cigarette Smoke Affects Keratinocytes SRB1 Expression and Localization via H2O2 Production and HNE Protein Adducts Formation. Plos One 7 (2012): e33592.
- Caliri A, Tommasi S, Besaratinia A. Relationships among smoking, oxidative stress, inflammation, macromolecular damage, and cancer. Mutation Research/Reviews in Mutation Research 787 (2021): 108365.
- Wang Z, Zhang M. Smoking and the risk of atopic dermatitis: A two-sample mendelian randomization study. Medicine 102 (2023): e36050.
- Graif Y, German L, Ifrah A, et al. Dose-response association between smoking and atopic eczema: results from a large cross-sectional study in adolescents. Dermatology 226 (2013): 195-199.
- Alturki B, Almutairi R, Al-mutairi A, et al. The Effects of Smoking on the Severity of Atopic Dermatitis in Saudi Arabia. Cureus 15 (2023): e50315.
- Kim S, Sim S, Choi H. Atopic dermatitis is associated with active and passive cigarette smoking in adolescents. Plos One 12 (2017): e0187453.
- Chao L, Liang W, Zhao X, et al. Maternal tobacco exposure during pregnancy and atopic dermatitis in offspring: A systematic review and meta-analysis. Journal of the European Academy of Dermatology and Venereology 38 (2024): 1947-1953.
- Wang I, Hsieh W, Wu K, et al. Effect of gestational smoke exposure on atopic dermatitis in the offspring. Pediatric Allergy and Immunology 19 (2008): 580-586.
- Shinohara M, Matsumoto K. Fetal Tobacco Smoke Exposure in the Third Trimester of Pregnancy Is Associated with Atopic Eczema/Dermatitis Syndrome in Infancy. Pediatric Allergy, Immunology, and Pulmonology 30 (2017): 155-162.
- Lau H, Lee J, Yap Q, et al. Smoke exposure and childhood atopic eczema and food allergy: A systematic review and meta-analysis. Pediatric Allergy and Immunology 34 (2023): e14010.
- Kantor R, Silverberg J. Environmental risk factors and their role in the management of atopic dermatitis. Expert Review of Clinical Immunology 13 (2016): 15-26.
- Silverberg J, Hanifin J, Simpson E. Climatic factors are associated with childhood eczema prevalence in US. Journal of Investigative Dermatology 133 (2013): 1752-1759.
- Weiland S, Husing A, Strachan D, et al. Climate and the prevalence of symptoms of asthma, allergic rhinitis, and atopic eczema in children. Occupational & Environmental Medicine 61 (2004): 609-615.
- Quirk SK, Rainwater E, Shure AK, et al. Vitamin D in atopic dermatitis, chronic urticaria and allergic contact dermatitis. Expert Rev Clin Immunol. 2016 Aug;12(8):839-47.
- Frieri M, Valluri A. Vitamin D deficiency as a risk factor for allergic disorders and immune mechanisms. Allergy and Asthma Proceedings 32 (2011): 438-444.
- Peroni D, Piacentini G, Cametti E, et al. Correlation between serum 25-hydroxyvitamin D levels and severity of atopic dermatitis in children. British Journal of Dermatology 164 (2011): 1078-1082.
- Sargen M, Hoffstad O, Margolis D. Warm, Humid, and High Sun Exposure Climates are Associated with Poorly Controlled Eczema: PEER (Pediatric Eczema Elective Registry) Cohort, 2004-2012. Journal of Investigative Dermatology 134 (2014): 51-57.
- Langan S, Bourke J, Silcocks P, et al. An exploratory prospective observational study of environmental factors exacerbating atopic eczema in children. British Journal of Dermatology 154 (2006): 979-980.
- Kubo A, Nagao K, Amagai M. Epidermal barrier dysfunction and cutaneous sensitization in atopic diseases. The Journal of Clinical Investigation 122 (2012): 440-447.
- Sato J, Denda M, Chang S, et al. Abrupt decreases in environmental humidity induce abnormalities in permeability barrier homeostasis. Journal of Investigative Dermatology 119 (2002): 900-904.
- Denda M, Sato J, Tsuchiya T, et al. Low humidity stimulates epidermal DNA synthesis and amplifies the hyperproliferative response to barrier disruption: implication for seasonal exacerbations of inflammatory dermatoses. Journal of Investigative Dermatology 111 (1998): 873-878.
- Ashida Y, Ogo M, Denda M. Epidermal interleukin-1 alpha generation is amplified at low humidity: implications for the pathogenesis of inflammatory dermatoses. British Journal of Dermatology 144 (2001): 238-243.
- Engebretsen K, Johansen J, Kezic S, et al. The effect of environmental humidity and temperature on skin barrier function and dermatitis. Journal of the European Academy of Dermatology and Venereology 30 (2015): 223-249.
- Macchione M, Yoshizaki K, Frias D, et al. Fragrances as a trigger of immune responses in different environments. Toxicology in Vitro 96 (2024): 105769.
- Johansen J. Fragrance contact allergy: a clinical review. American Journal of Clinical Dermatology 4 (2012): 789-798.
- Van Amerongen C, Ofenloch R, Cazzaniga S, et al. Skin exposure to scented products used in daily life and fragrance contact allergy in the European general population - The EDEN Fragrance Study. Contact Dermatitis 84 (2021): 385-394.
- Kwangsukstith C, Maibach H. Effect of age and sex on the induction and elicitation of allergic contact dermatitis. Contact Dermatitis 33 (1995): 289-298.
- Modjtahedi B, Modjtahedi S, Maibach H. The sex of the individual as a factor in allergic contact dermatitis. Contact Dermatitis 50 (2004): 53-59.
- Nemeth D, Temesvari E, Hollo P, et al. Preservative Contact Hypersensitivity among Adult Atopic Dermatitis Patients. Life 12 (2022): 715.
- Travassos A, Claes L, Boey L, et al. Non-fragrance allergens in specific cosmetic products. Contact Dermatitis 65 (2011): 276-285.
- Quiros-Alcala L, Hansel N, McCormack M, et al. Paraben exposures and asthma-related outcomes among children from the US general population. The Journal of Allergy and Clinical Immunology 143 (2019): 948-956.
- Chalubinski M, Kowalski M. Endocrine disrupters – potential modulators of the immune system and allergic response. Allergy 61 (2006): 1326-1335.
- Jackson-Browne M, Henderson N, Patti M, et al. The Impact of Early-Life Exposure to Antimicrobials on Asthma and Eczema Risk in Children. Current Environmental Health Reports 6 (2019): 214-224.
- Arafune J, Tsujiguchi H, Hara A, et al. Increased Prevalence of Atopic Dermatitis in Children Aged 0-3 Years Highly Exposed to Parabens. International Journal of Environmental Research and Public Health 18 (2021): 11657.
- Thurmann L, Herberth G, Seiwert B, et al. Prenatal paraben exposure and atopic dermatitis-related outcomes among children. Allergy 76 (2021): 3122-3132.
- Vindenes H, Svanes C, Lygre S, et al. Exposure to environmental phenols and parabens, and relation to body mass index, eczema and respiratory outcomes in the Norwegian RHINESSA study. Environmental Health 20 (2021): 81.
- Solomon I, Ilie M, Draghici C, et al. The impact of lifestyle factors on evolution of atopic dermatitis: An alternative approach. Experimental and Therapeutic Medicine 17 (2018): 1078-1084.
- Worthen M, Cash E. Stress Management. StatPearls Publishing. Published online January 2025.
- Dhar S, Malakar R, Banerjee R, et al. An Uncontrolled Open Pilot Study to Assess the Role of Dietary Eliminations in Reducing the Severity of Atopic Dermatitis in Infants and Children. Indian Journal of Dermatology 54 (2009): 183-185.
- Uenishi T, Sugiura H, Uehara M. Role of foods in irregular aggravation of atopic dermatitis. The Journal of Dermatology 30 (2014): 91-97.
- Zhang J, Loman L, Oldhoff M, et al. Association between moderate to severe atopic dermatitis and lifestyle factors in the Dutch general population. Clinical and Experimental Dermatology 47 (2022): 1523-1535.
- Zhang Y, Heinemann N, Rademacher F, et al. Skin Care Product Rich in Antioxidants and Anti-Inflammatory Natural Compounds Reduces Itching and Inflammation in the Skin of Atopic Dermatitis Patients. Antioxidants 11 (2022): 1071.
- Dumbuya H, Podimatis K, Kerob D, et al. Efficacy of a Prebiotic Skincare Regimen on Improving Mild Atopic Dermatitis and Severe Xerosis in Diverse Ethnically Patients. J Drugs Dermatol 23 (2024): SF395747s12-SF395747s22
- Butala S, Paller A. Optimizing topical management of atopic dermatitis. Annals of Allergy, Asthma & Immunology 128 (2022): 488-504.
- Fleischer D, Udkoff J, Borok J, et al. Atopic dermatitis: skin care and topical therapies. Semin Cutan Med Surg 36 (2017): 104-110.
- Sala-Cunill A, Lazaro M, Herraez L, et al. Basic Skin Care and Topical Therapies for Atopic Dermatitis: Essential Approaches and Beyond. Journal of Investigational Allergology and Clinical Immunology 28 (2018): 379-391.
- Bawany F, Northcott C, Beck L, et al. Sleep Disturbance and Atopic Dermatitis: Relationships, Methods for Assessment, and Therapies. The Journal of Allergy and Clinical Immunology 9 (2021): 1488-1500.
- Mindell J, Leichman E, Parikh-Das A, et al. Sleep improvements following atopic dermatitis management in young children. Sleep Health 10 (2024): 209-212.